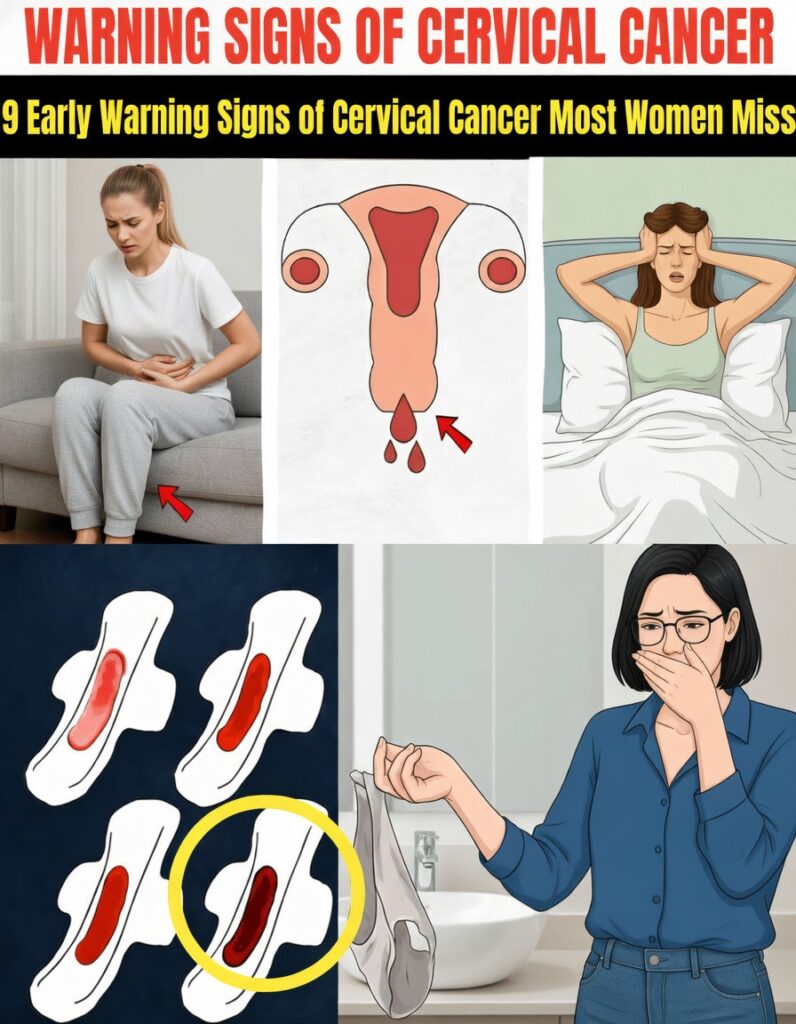
Understanding Cervical Cancer
Cervical cancer starts in the cells lining the cervix, the lower, narrow part of the uterus that opens into the vagina. Large health organizations, including the World Health Organization (WHO), agree that long‑lasting infection with certain high‑risk types of human papillomavirus (HPV) is the leading cause in most cases.
One of the biggest challenges is that early cervical cancer usually produces no obvious symptoms. In the beginning, changes in cervical cells often go unnoticed, which is why many women are diagnosed only after the disease has progressed.
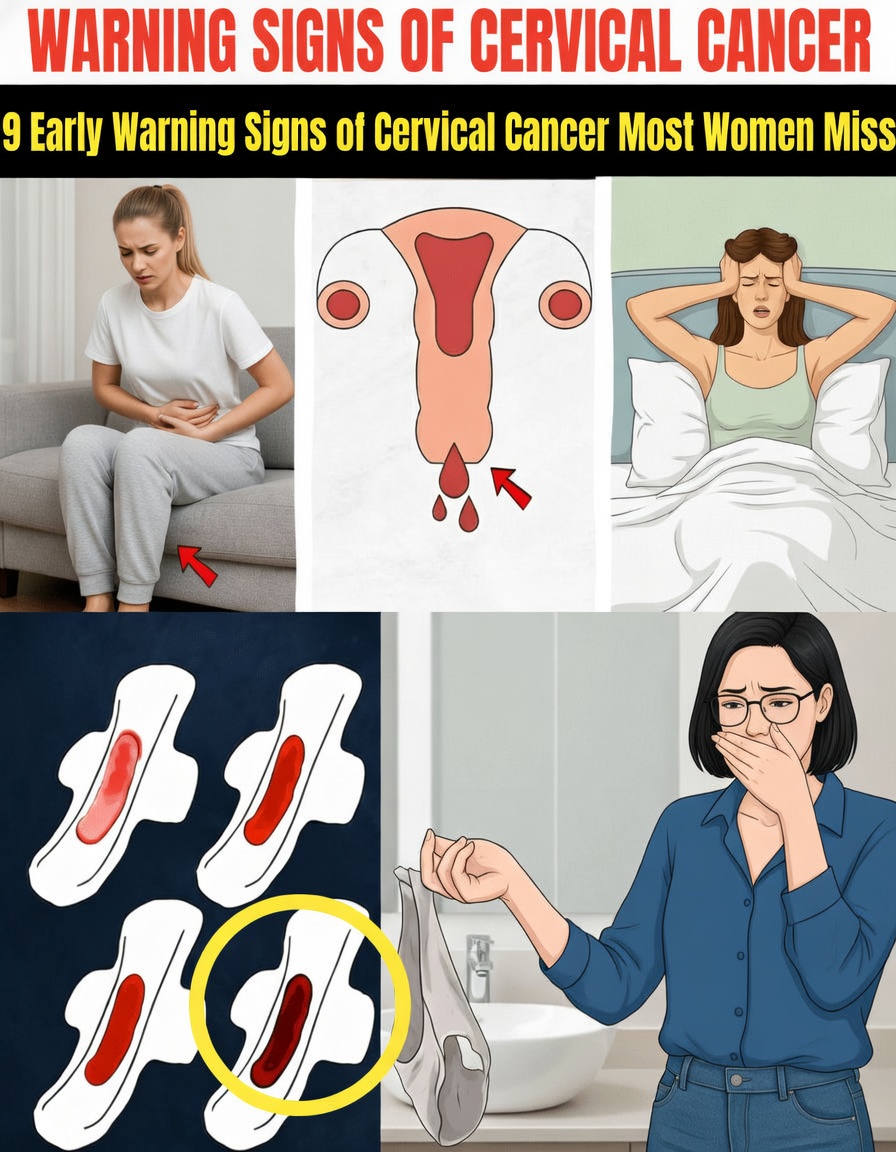
Because of this, regular screening with Pap tests and HPV tests is still the most reliable way to detect precancerous changes before they turn into cancer. At the same time, knowing potential warning signs can help you seek medical advice sooner.
Below are some commonly overlooked cervical cancer symptoms that should not be ignored, especially if they persist or get worse over time.
9 Cervical Cancer Warning Signs That Often Go Unnoticed
These nine possible signs are frequently mistaken for “normal” issues or other conditions. They can be caused by non‑cancerous problems as well, but ongoing or unexplained changes always deserve medical evaluation.
1. Unusual Vaginal Bleeding
According to organizations such as the American Cancer Society and the Mayo Clinic, this is one of the most frequent early warning signs.
Unusual bleeding may include:
- Spotting or bleeding between menstrual periods
- Bleeding after sexual intercourse
- Bleeding after menopause
- Periods that suddenly become much heavier or last longer than usual
Any new or unexpected pattern of bleeding is reason to talk with a healthcare professional.
2. Abnormal Vaginal Discharge
A change in vaginal discharge can also signal a problem. Warning features include:
- Watery or very thin discharge that is new or unusual for you
- Discharge that is bloody, pink, brown, or streaked with blood
- A strong or foul odor that is not typical for your normal cycle
Discharge that looks different and keeps recurring should be checked.
3. Pain During or After Sex
Pain or discomfort during intercourse (dyspareunia) is not something to ignore. It may feel like:
- Deep pelvic pain with penetration
- Sharp or aching pain during or after sex
This symptom can be related to irritation, inflammation, or abnormal growths in or around the cervix.
4. Persistent Pelvic or Lower Back Pain
Ongoing pain in the lower abdomen, pelvis, or lower back without a clear cause can sometimes occur as cervical disease advances. You might notice:
- A constant dull ache
- Intermittent cramping or pressure
- Pain not linked to your usual menstrual cramps or to an injury
If pelvic or back pain is persistent and unexplained, it’s worth discussing with your doctor.
5. Swelling or Pain in the Legs
In more advanced cases, the cancer can press on nearby structures, including blood vessels and lymphatic channels. This may lead to:
- Swelling in one or both legs
- A heavy or tight feeling in the legs
- Leg pain that does not improve with rest
While this is less common, it is important to evaluate persistent swelling or pain.
6. Unexplained Fatigue or Weight Loss
General symptoms like:
- Feeling extremely tired despite adequate rest
- Losing weight without changing diet or exercise
can appear in later stages and often occur along with other symptoms such as abnormal bleeding or pain.
7. Frequent or Painful Urination
When nearby tissues are involved, you might notice urinary changes, such as:
- Burning or pain during urination
- Needing to urinate more often than usual
- Difficulty emptying the bladder completely
These signs are also common in infections, but if they don’t resolve, they should be evaluated.
8. Changes in Bowel Habits
If cervical cancer spreads to surrounding areas, it can sometimes affect the bowel, leading to:
- New or persistent constipation
- Ongoing diarrhea without clear cause
- Blood in the stool
Any lasting change in bowel habits or rectal bleeding should be promptly checked.
9. Itching or Burning in the Vaginal Area
Persistent irritation is another symptom sometimes mentioned in medical resources. This can involve:
- Constant itching that does not improve with usual treatments
- Burning or soreness around the vaginal opening
- Ongoing irritation without a clear explanation
Because infections and skin conditions can look similar, persistent symptoms always warrant a professional assessment.
Normal Changes vs. Possible Warning Signs
Many of these symptoms overlap with more common issues, such as infections, hormonal changes, or side effects of contraception. The key difference is persistence, severity, or a clear change from your normal pattern.
-
Typical variations
- Occasional mild spotting
- Mild cramps around your period
- Discharge that changes slightly with your cycle but has no strong odor
-
Potential red flags
- Bleeding after sex or after menopause
- Bleeding between periods that is new or recurring
- Foul‑smelling, watery, or bloody discharge
- Pain that interferes with daily activities or sexual health
If any of these concerning signs last longer than two weeks or keep returning, make an appointment with a healthcare provider rather than waiting for them to go away on their own.
Why Cervical Cancer Symptoms Are Often Missed
Many women lead busy lives and may dismiss symptoms as “just stress”, “hormones”, or “normal aging.” Factors such as:
- Hormonal fluctuations
- Birth control methods
- Everyday stress
- Common infections
can imitate some of the same cervical cancer symptoms, making it easy to overlook early warning signs.
Experts at organizations like the CDC and the National Cancer Institute (NCI) emphasize that early cervical changes are usually silent. This is exactly why routine screening is so important: Pap tests and HPV tests can detect abnormal cells long before symptoms appear, when treatment is most effective.
At the same time, research shows that HPV vaccination, combined with regular screening, has significantly lowered cervical cancer rates in many countries. Staying alert to changes in your body is another powerful layer of protection.
Practical Steps to Protect Your Cervical Health

You can take several simple but impactful actions to reduce your risk and catch problems early:
1. Keep Up With Regular Screenings
Follow age‑appropriate guidelines or your doctor’s recommendations, for example:
- For many women aged 30–65 at average risk, an HPV test every 5 years (or a Pap test schedule recommended by your provider)
- In some places, self-collection options for HPV testing are available
Screening intervals may differ based on your medical history, prior results, and local guidelines.
2. Pay Attention and Track Symptoms
Use a notebook or a health app to record:
- Episodes of unusual bleeding
- Changes in discharge
- Pelvic, back, or leg pain
- Urinary or bowel changes
A brief symptom log can help your healthcare provider quickly see patterns and decide on appropriate tests.
3. Get HPV Vaccinated if You Are Eligible
The HPV vaccine protects against the most common high‑risk HPV types linked to cervical cancer and other cancers. Even if you are already sexually active, vaccination may still offer benefits, depending on your age and situation.
4. Practice Safe and Healthy Habits
Lifestyle factors also influence risk:
- Use barrier protection (such as condoms) during sex to reduce HPV and other STI exposure
- Avoid smoking, which increases the chance of cervical cell changes
- Maintain a balanced diet, regular exercise, and stress management to support overall immune health
5. Know What Is “Normal” for You
Every body is different. Notice your usual:
- Menstrual patterns
- Discharge quantity and texture
- Typical level of discomfort (if any) around your period
The more familiar you are with what’s normal, the easier it is to recognize when something is off and needs medical attention.
Prevention and Early Detection: The Real “Secret”
The most powerful tool against cervical cancer is not discovering a rare symptom—it is consistent, high‑quality screening and vaccination.
According to WHO and other major health organizations:
- Cervical cancer is highly preventable when precancerous changes are found and treated early.
- Many women who follow recommended Pap and HPV testing schedules never develop advanced disease.
When you combine:
- Routine screening
- HPV vaccination (if eligible)
- Awareness of possible warning signs
you greatly increase your chances of catching any problem early—or preventing it altogether.
Frequently Asked Questions
What is the most common early sign of cervical cancer?
Abnormal vaginal bleeding—such as bleeding after intercourse, between periods, or after menopause—is often cited by experts as one of the earliest noticeable warning signs. However, early cervical cancer may cause no symptoms at all, which is why routine screening is essential.
Can cervical cancer be prevented?
Cervical cancer can often be prevented or caught very early through:
- HPV vaccination
- Regular Pap and/or HPV tests
- Treating precancerous changes promptly
- Avoiding smoking and practicing safer sex
No method is 100% protective, but these steps significantly lower your risk.
When should I see a doctor about possible cervical cancer symptoms?
You should see a healthcare provider if you experience:
- Any new or unusual vaginal bleeding (especially after sex or after menopause)
- Persistent or foul‑smelling vaginal discharge
- Ongoing pelvic, back, or leg pain
- Lasting changes in urination or bowel habits
- Vaginal itching, burning, or discomfort that does not improve
If something feels wrong or different and lasts more than a couple of weeks, do not wait—schedule a medical evaluation. Early assessment provides clarity and, if needed, timely treatment.