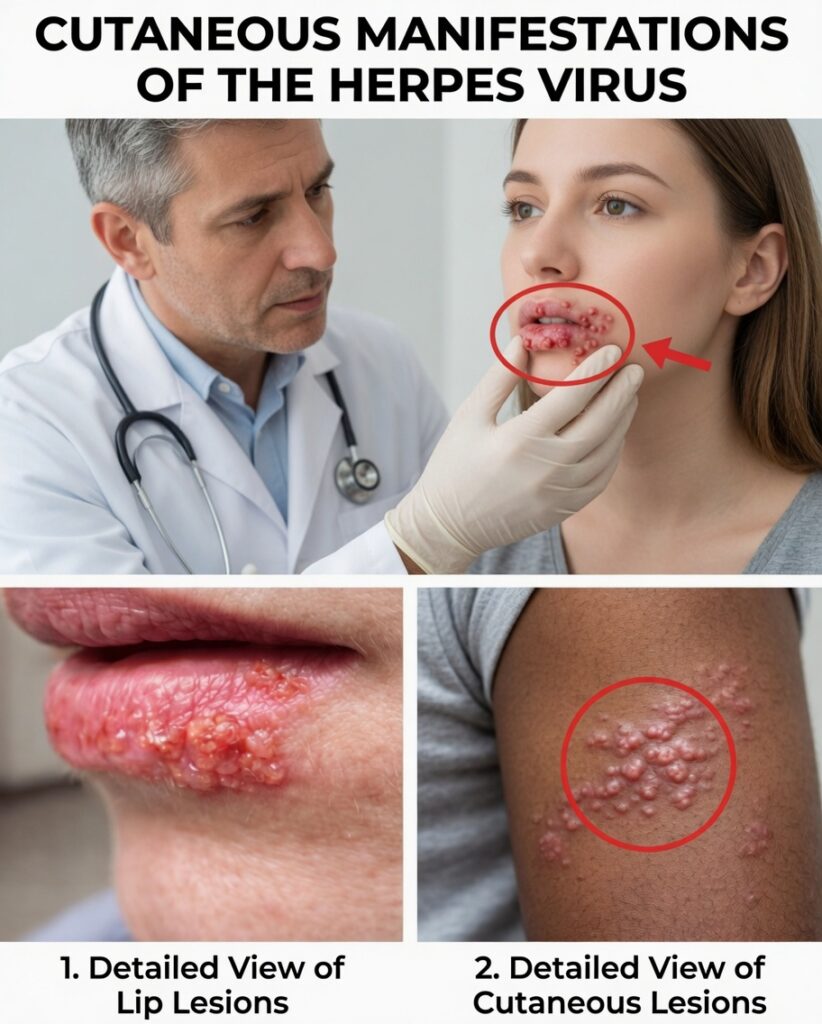
Herpes Keeps Coming Back? What Truly Reactivates the Virus—and How Many People Are Cutting Outbreaks Dramatically
Recurring blisters or sores on the lips or in the genital area are more common than many people realize. At first, it’s easy to dismiss them as an allergy, an irritated pimple, stress, or a temporary skin issue. The lesions appear, cause discomfort for a few days (sometimes weeks), then fade away… only to return months later.
This repeating pattern can lead to embarrassment, fear around intimacy, and constant worry about when the next episode will strike. Millions of adults live with the herpes simplex virus (HSV), and many don’t even know they carry it. The encouraging news: with the right understanding and practical strategies, many people can significantly lower both the frequency and severity of outbreaks—often improving quality of life in a meaningful way.
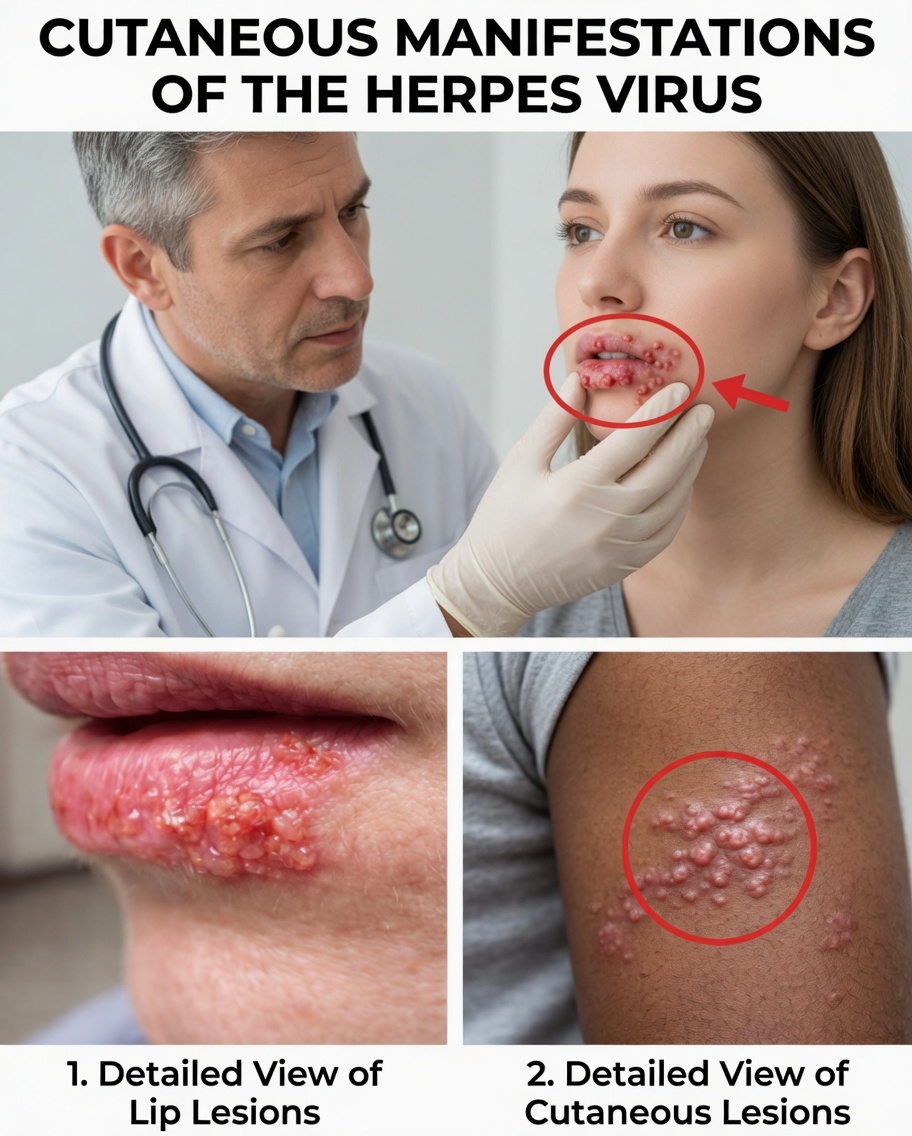
Why Do These Blisters Keep Returning?
Herpes simplex is usually discussed in two main types:
- HSV-1, most often linked to oral herpes (cold sores)
- HSV-2, most often linked to genital herpes (though either type can affect either area)
After the first infection—which may be mild or unnoticed—the virus does not leave the body. Instead, it travels along nerves and stays dormant (inactive) in nerve cells near the spine or facial region.
At certain times, HSV can reactivate. When that happens, the virus travels back to the skin or mucous membranes and can cause familiar symptoms such as:
- tingling, itching, or burning (often an early warning sign)
- redness
- small fluid-filled blisters
- pain or tenderness
- crusting as the area heals
Most people with HSV experience recurrences at some point. For some, outbreaks happen several times a year; for others, they are rare.
The effects are not only physical. Many people report reduced self-esteem, fear of rejection, and ongoing anxiety about transmission. In fact, the emotional burden can feel heavier than the physical discomfort.
Hidden Triggers That Can Reactivate HSV
Outbreaks rarely happen “for no reason.” Reactivation is often linked to specific triggers, including:
- High stress levels
Elevated cortisol during intense stress may temporarily weaken immune defenses. - Sun exposure or skin irritation
Sunburned lips or friction/irritation in the genital area can increase the chance of lesions. - Hormonal shifts
Some women notice outbreaks around their menstrual cycle. - Lowered immunity
Illness, poor sleep, and nutritional deficiencies can make the body more vulnerable.
A practical way to uncover your patterns is to track dates, symptoms, lifestyle factors, and possible triggers—many people discover clear trends over time.
What Your Body May Be Signaling During Recurrences
Frequent or recurring outbreaks often highlight a few key realities:
- the virus remains present in nearby nerve cells
- the immune system may have dipped temporarily
- early symptoms (tingling/itching) often act as a warning that an outbreak is starting
- stress and fatigue commonly play a major role
- sleep habits, nutrition, and sun exposure can influence outbreak frequency
Recognizing these signals early can help you respond sooner and potentially reduce the intensity of an episode.
Evidence-Based Strategies to Reduce Outbreaks
There are effective, widely used approaches that help many people manage recurrent herpes.
- Suppressive antiviral therapy
When recommended by a clinician, daily antiviral medication may substantially reduce outbreak frequency. - Early treatment at the first warning signs
Starting care as soon as tingling or burning begins often shortens the outbreak and reduces symptom severity. - Lifestyle habits that support immune health
- Aim for at least 7 hours of sleep per night
- Maintain a balanced, nutrient-rich diet
- Use stress-management tools such as exercise, meditation, or therapy
- Protect lips with SPF lip balm, especially with strong sun exposure
These steps can help the body keep HSV dormant for longer periods.
A Realistic Path Toward Better Control
Many people who once had frequent outbreaks see major improvement after they:
- identify personal triggers,
- strengthen daily health habits,
- and get appropriate medical guidance.
Over time, what once felt unpredictable can become manageable. Anxiety often decreases, confidence improves, and intimate relationships can feel comfortable again.
Practical Steps You Can Take Right Now
- Schedule an appointment with a doctor or sexual health clinic
- Track how often outbreaks occur, how long they last, and what may have triggered them
- If possible, take a photo of an active lesion to support accurate evaluation
- Discuss prevention and treatment options, including episodic vs. suppressive antiviral therapy
Small actions like these can make a meaningful difference.
Frequently Asked Questions
-
How can I know if it’s really herpes?
Only a healthcare professional can confirm HSV through appropriate testing and evaluation. -
Is there a cure?
There is currently no definitive cure, but there are effective treatments to manage symptoms and reduce recurrences. -
Can you have a relationship if you have herpes?
Yes. With open communication, appropriate protection, and medical guidance, transmission risk can be significantly reduced.
Disclaimer
This article is for informational purposes only and does not replace professional medical advice. Any recurring lesion should be assessed by a qualified healthcare provider for proper diagnosis and treatment.