Don’t Ignore These Signs: Acting Early Can Protect Your Health
Many women go through daily life without realizing that subtle body changes can point to something more serious. Cervical cancer often develops quietly in its early stages, with little to no obvious symptoms. That’s why some cases are detected later than ideal. Even though doctors recommend routine screening, unusual symptoms are still frequently mistaken for hormonal fluctuations or “normal” menstrual discomfort.
The encouraging news is that paying attention to your body can make a real difference. Recognizing early warning signs may help you seek care sooner and improve the chances of effective treatment. Below are 9 cervical cancer warning signs that are commonly overlooked—but deserve attention.
Why Early Detection Can Be Difficult
Cervical cancer begins in the cells of the cervix, the lower part of the uterus that connects to the vagina. In the beginning, it typically causes no symptoms. When signs do appear, they can be mild and easily confused with infections, hormonal changes, or other common conditions.
9 Warning Signs You Shouldn’t Ignore
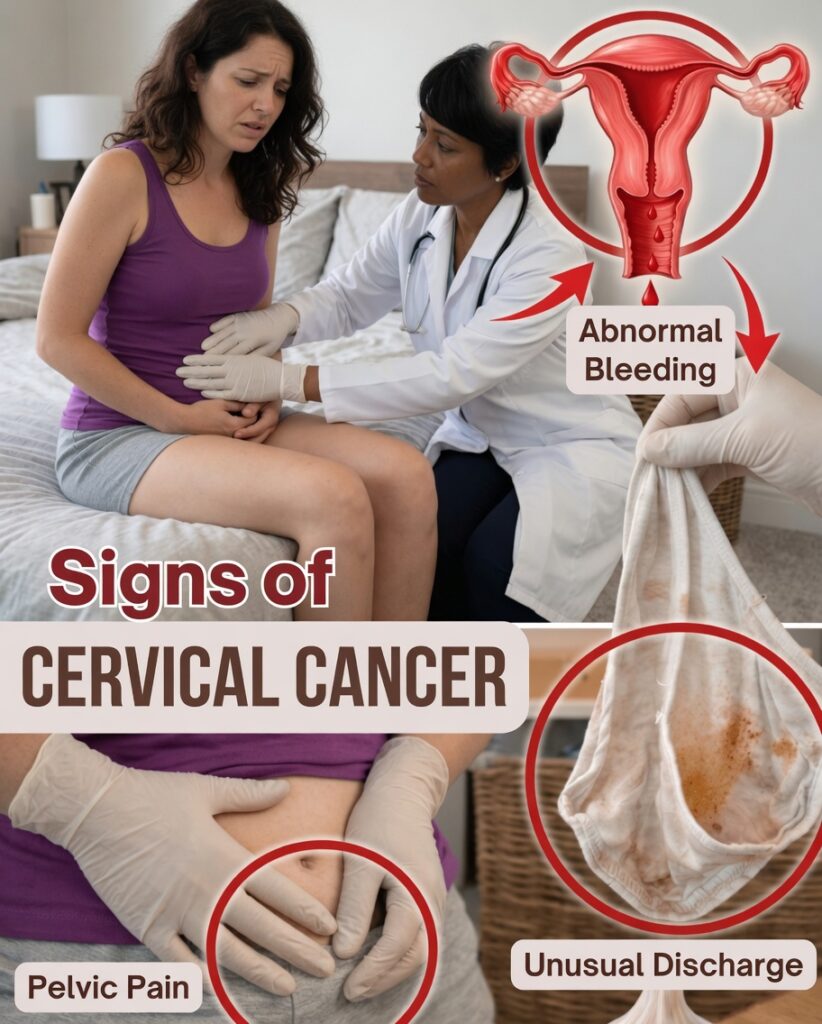
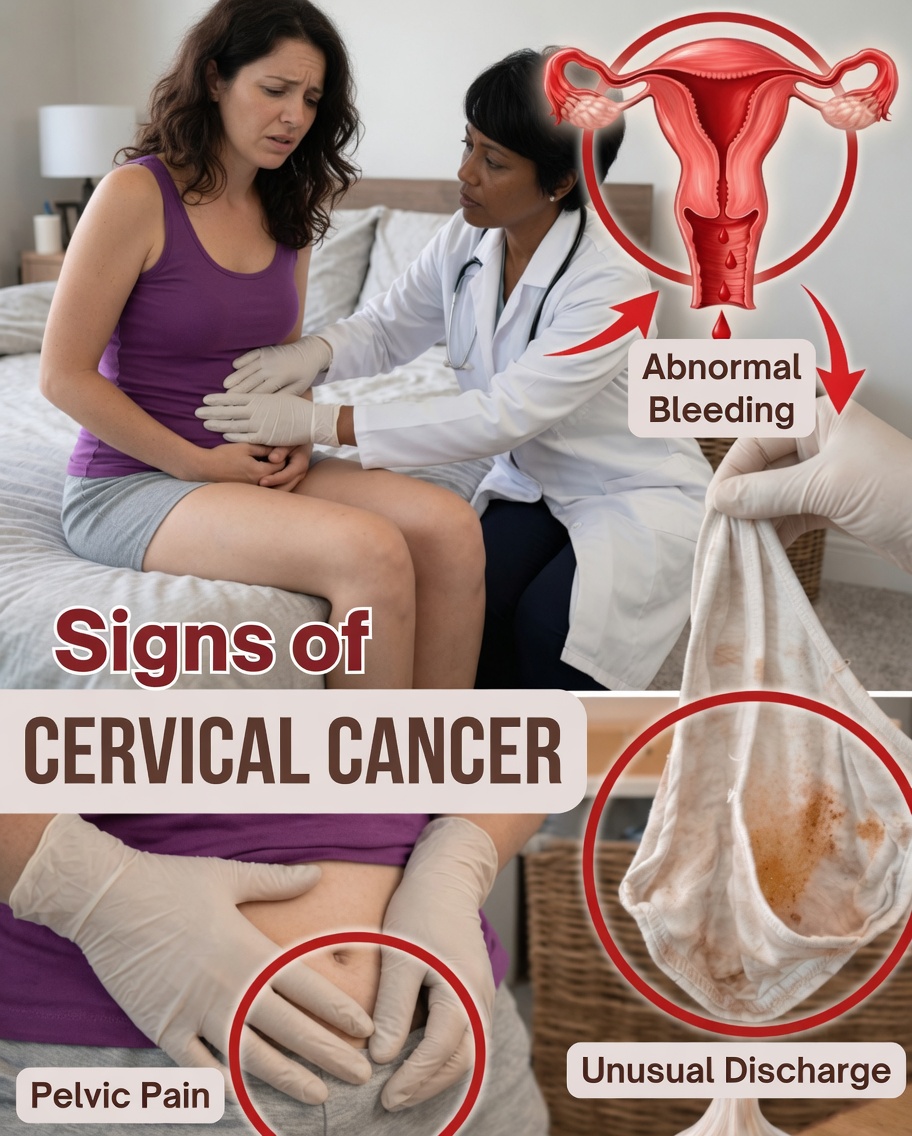
1. Unusual vaginal bleeding
Bleeding between periods, after sex, heavier-than-usual periods, or any bleeding after menopause can be important signals.
2. Abnormal vaginal discharge
Discharge that changes in smell, contains blood, appears unusual in color, or becomes more frequent/heavier should be checked.
3. Pain during or after sex
Pain or discomfort isn’t something you should simply “put up with.” It may be linked to changes in the cervix that need evaluation.
4. Ongoing pelvic pain
Persistent pain in the lower abdomen/pelvic area, especially when it doesn’t match your menstrual cycle, can be a warning sign.
5. Heavier or longer periods than normal
If your period suddenly becomes much heavier or lasts more days than usual, it’s worth investigating.
6. Bleeding after menopause
Any postmenopausal bleeding is abnormal and should be assessed promptly.
7. Unexplained, persistent fatigue
Extreme tiredness without a clear cause can occur with various health issues—especially when combined with other symptoms.
8. Lower back or leg pain
Ongoing pain in the lower back or legs can appear as the condition progresses and should not be ignored.
9. Urinary or bowel changes
Trouble urinating, blood in urine, or noticeable bowel changes may occur, particularly in more advanced stages.
Normal Changes vs. Concerning Symptoms
Often normal:
- Occasional light spotting
- Mild cramps
- Slight, temporary changes in discharge
More concerning:
- Frequent bleeding outside your cycle
- Persistent or worsening pain
- Discharge with strong odor or blood
If something feels “off” for more than two weeks, don’t dismiss it.
What You Can Do Right Now
- Get routine cervical screening (Pap smear and/or HPV test, as recommended)
- Consider the HPV vaccine if it’s appropriate for you
- Track and write down any changes in symptoms
- Support your health with strong daily habits (balanced diet, regular movement, avoid smoking)
- See a healthcare professional if symptoms persist or worsen
What to Expect at a Medical Appointment
A clinician may perform a physical and pelvic exam and recommend tests such as a Pap test, HPV testing, or additional procedures if needed. In many cases, results do not indicate cancer—but getting checked provides clarity and peace of mind.
Frequently Asked Questions
What causes cervical cancer?
The most common cause is persistent infection with high-risk HPV (human papillomavirus), a very common virus transmitted through intimate contact.
Can cervical cancer be prevented?
In many cases, yes. HPV vaccination, regular screening, and proactive healthcare significantly reduce the risk.
How often should I get screened?
Guidelines vary by country and individual risk. Screening often begins around ages 21–25, then typically every 3–5 years, depending on the type of test and medical advice.
Final Thoughts
Knowing these signs doesn’t mean you have cervical cancer—it means you’re prepared. Awareness and early action can save lives. Small steps today can make a major difference for your future health.
Disclaimer: This content is for informational purposes only and does not replace medical advice. If you have symptoms or concerns, consult a qualified healthcare professional.