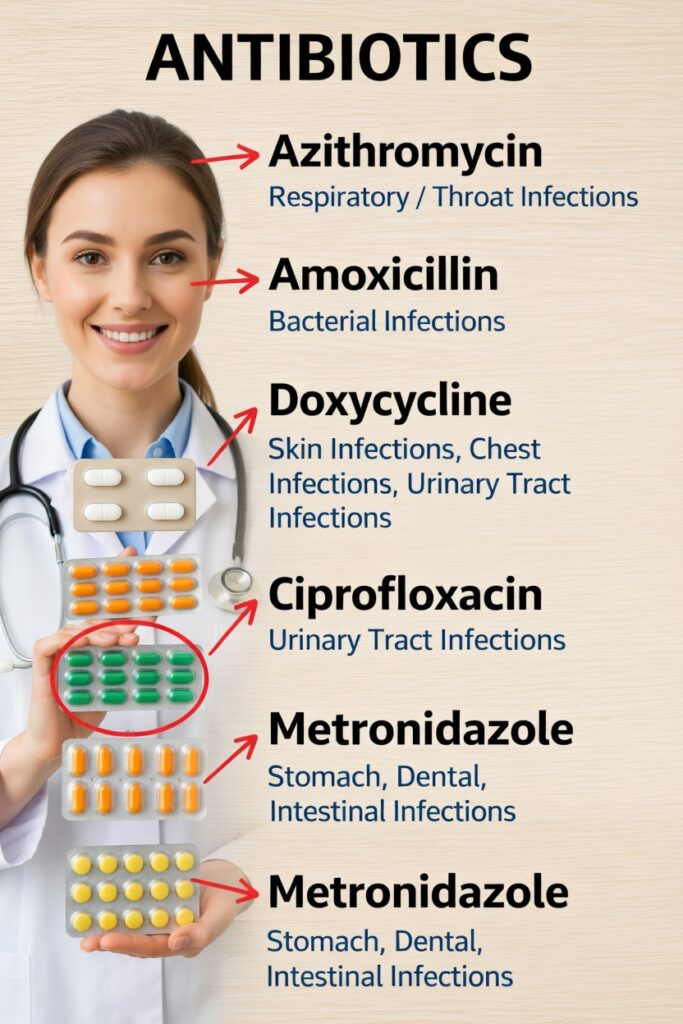
5 Common Antibiotics Explained: Uses, Differences, and Safe Practices
Many people experience bacterial infections each year—from sore throats and chest infections to skin issues or urinary tract infections. When used correctly, antibiotics can be an important part of treatment. Problems arise when they are used too often, taken incorrectly, or used when they’re not needed, which contributes to antibiotic resistance.
This guide looks at five widely used antibiotics—azithromycin, amoxicillin, doxycycline, ciprofloxacin, and metronidazole—so you can better understand how they are typically used and how to discuss them more confidently with a healthcare professional.
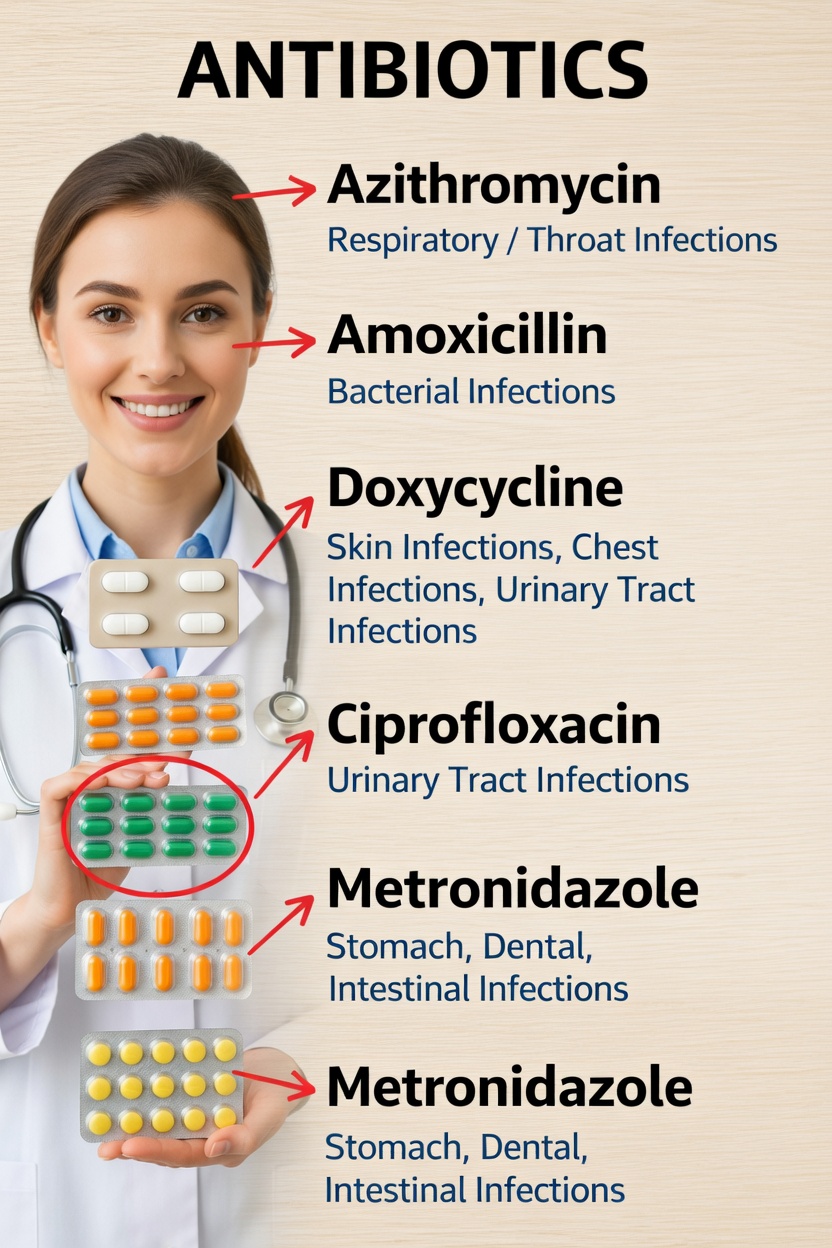
Understanding these basics is not about self-prescribing. Instead, it helps you ask clearer questions, understand why a doctor chooses one medicine over another, and use antibiotics more responsibly.
Why These 5 Antibiotics Are So Common
These medications appear frequently in prescriptions because they can target many everyday bacterial infections. Health organizations around the world consistently list them among the most discussed and commonly used antibiotics.
Knowing their usual roles makes it easier to see how doctors match each one to:
- The site of infection (lungs, skin, gut, urinary tract, etc.)
- The most likely bacteria involved
- The patient’s age, history, and allergies
Azithromycin: Often Chosen for Respiratory and Throat Infections
Azithromycin is a macrolide antibiotic often considered for certain upper and lower respiratory tract infections and throat-related bacterial illnesses.
Typical uses include:
- Some bacterial sore throats and tonsillitis (when appropriate)
- Certain community-acquired chest infections
- Selected sinus or ear infections (depending on guidelines)
Key points:
- It is often prescribed as a short course, which many patients find convenient.
- Research shows macrolides like azithromycin can help manage community-acquired respiratory infections when bacteria are involved.
- Some people report symptom relief—such as reduced cough or airway inflammation—within a few days, though full recovery may take longer.
Because it has relatively broad activity, azithromycin is also used in specific conditions outlined in clinical guidelines, but always under medical supervision.
Amoxicillin: A First-Line Option for Many Everyday Infections
Amoxicillin, a member of the penicillin family, is one of the most widely prescribed antibiotics globally. It is commonly selected for a variety of straightforward bacterial infections, for example:
- Ear infections (otitis media)
- Sinus infections (sinusitis)
- Certain skin and soft tissue infections
- Some dental infections
What makes amoxicillin stand out:
- Penicillins are often first-line choices for uncomplicated cases because of their long safety record and well-understood effectiveness.
- Amoxicillin is available in multiple forms (such as liquid suspensions, capsules, and tablets), which makes dosing easier for both children and adults.
- It is versatile, but still needs to be matched to the most likely bacteria and the site of infection, not used as a one-size-fits-all solution.
Doxycycline: Broad Coverage for Skin, Chest, and Urinary Problems
Doxycycline is part of the tetracycline class and is valued for its broad-spectrum activity. It is often used when several different bacteria could be responsible, and common uses include:
- Acne and other chronic skin conditions
- Certain respiratory infections, including some forms of pneumonia or bronchitis
- Selected urinary tract infections (UTIs), depending on local guidance
- Some infections related to outdoor exposure (for example, tick-borne diseases, in line with regional protocols)
Why doxycycline is considered versatile:
- Tetracyclines provide wide coverage against various bacteria, making doxycycline useful in situations where the exact organism is not yet confirmed.
- It can be used alone or in combination with other antibiotics, depending on the infection.
- It often features in treatment plans for long-term skin issues or specific travel-related or environmental exposures.
Ciprofloxacin: Frequently Associated with Urinary Tract Infections
Ciprofloxacin is a fluoroquinolone antibiotic often linked with the treatment of urinary tract infections (UTIs). It targets many of the bacteria that commonly cause infections of the urinary system.
Where it typically fits in:
- Certain uncomplicated or complicated UTIs
- Some gastrointestinal and other infections, when recommended by guidelines
Important considerations:
- Major health authorities emphasize that fluoroquinolones should be used carefully and selectively, especially for UTIs, because of potential side effects and emerging resistance.
- In some regions, ciprofloxacin is reserved for situations where other antibiotics are not suitable or have failed.
- Its use illustrates how antibiotic choices shift over time due to resistance patterns and updated safety information.
Metronidazole: A Specialist for Gut, Dental, and Anaerobic Infections
Metronidazole is especially effective against anaerobic bacteria (organisms that thrive in low-oxygen environments) and some parasites. It plays a key role in infections involving:
- The gastrointestinal tract (for example, certain intestinal infections)
- Dental and gum infections, including dental abscesses
- Abdominal and pelvic infections where anaerobic bacteria are suspected
Why metronidazole is important:
- Research supports its use in mixed infections where oxygen-poor environments favor anaerobic bacteria.
- It often appears in treatment protocols for gut, dental, and intra-abdominal infections, sometimes combined with other antibiotics.
- Its focused activity shows that antibiotics are not interchangeable—different agents are designed for different types of bacteria.
Quick Overview: How These Antibiotics Compare
Here is a concise comparison of their typical roles:
- Azithromycin – Often used for respiratory and throat infections; usually shorter treatment courses.
- Amoxicillin – A common first-line option for everyday infections (ears, sinuses, skin, some dental issues).
- Doxycycline – Broad coverage for skin problems, some chest infections, and selected urinary issues.
- Ciprofloxacin – Frequently associated with urinary tract infections; used thoughtfully due to resistance and safety concerns.
- Metronidazole – Targets anaerobic bacteria; commonly used for intestinal, dental, and abdominal infections.
Key factors that influence which antibiotic a doctor chooses:
- Location of the infection (lungs, urinary tract, skin, gut, mouth, etc.)
- Suspected bacteria based on symptoms, tests, and local patterns
- Patient history, including allergies, previous reactions, and other medications
- Local resistance data, which inform which drugs are still likely to work
Why Learning About Common Antibiotics Matters
Antibiotic resistance occurs when bacteria adapt and antibiotics become less effective. This process is accelerated by overuse, misuse, or incomplete courses of treatment. Organizations such as the CDC stress that using antibiotics wisely is essential to preserve their effectiveness.
Understanding some basics helps you to:
- Recognize that antibiotics work against bacteria, not viruses (such as most colds and the flu).
- Avoid using antibiotics without clear medical advice.
- Support treatment success by following instructions correctly.
Studies show that when people are better informed about antibiotics, they are more likely to:
- Have productive discussions with healthcare providers
- Avoid unnecessary antibiotic requests
- Follow prescribed courses more carefully
Practical Tips for Responsible Antibiotic Use
You can support both your own health and global efforts against resistance by following these habits:
- Consult a healthcare professional before starting any antibiotic. Do not self-medicate, share medications, or use leftovers.
- Finish the full course exactly as prescribed, even if symptoms improve early.
- Ask questions, such as:
- “Is this infection likely bacterial or viral?”
- “Why was this specific antibiotic chosen?”
- “What side effects should I watch for, and when should I seek help?”
- Focus on prevention by:
- Washing hands regularly
- Covering coughs and sneezes
- Handling and cooking food safely
- Staying up to date with recommended vaccines
- Stay informed, because treatment guidelines and resistance patterns change over time.
Some people use probiotics during antibiotic treatment (on medical advice) to help support gut balance, although this is not a substitute for proper antibiotic use or professional guidance.
Conclusion: Use Knowledge to Guide Better Decisions
Azithromycin, amoxicillin, doxycycline, ciprofloxacin, and metronidazole are among the most frequently used antibiotics for common bacterial infections. Understanding their usual roles can help you:
- See why one drug may be chosen over another
- Ask better questions at medical appointments
- Use antibiotics more safely and effectively
The goal is not self-treatment, but informed partnership with your healthcare provider. Careful, responsible use today helps keep these medicines effective for you and for future patients.
Frequently Asked Questions
What should I do if antibiotics don’t seem to be working?
Contact your doctor promptly. Ongoing or worsening symptoms may mean the infection is not bacterial, the bacteria are resistant, or the treatment needs adjusting.
Can I drink alcohol while taking these antibiotics?
It depends on the specific medication. With metronidazole, alcohol is usually strongly discouraged due to potential reactions. Always check with your doctor or pharmacist about alcohol and any other drug interactions.
Are there natural alternatives to antibiotics?
Healthy habits such as rest, fluids, nutritious food, and good hygiene can support your immune system but do not replace antibiotics when a confirmed bacterial infection needs treatment. Always follow professional medical advice regarding when antibiotics are necessary.