Cervical Cancer Symptoms: Early Signs Every Woman Should Know
Imagine noticing a small change in your body, like light spotting between periods or unusual discharge, and assuming it is just stress, hormones, or a minor infection. Many women do exactly that. Unfortunately, symptoms that seem harmless can sometimes point to something more serious, including cervical cancer, a condition that affects thousands of women each year.
When warning signs are overlooked, fear and uncertainty can grow, and a problem that may have been easier to manage can become far more difficult. The good news is that recognizing symptoms early can help you take practical steps toward protecting your health. And before this article ends, you will learn about one unexpected symptom that often surprises even very observant women.
Why Recognizing Cervical Cancer Symptoms Early Matters
Cervical cancer can develop quietly, especially in its earliest stages. That is what makes it so easy to miss. According to the Mayo Clinic, noticeable symptoms often appear only after the disease has progressed, which is why awareness is so important.
Women who understand what to watch for are more likely to seek medical advice sooner. That early attention can make a meaningful difference and also reduce uncertainty. While no one can guarantee an outcome, staying informed, attending routine checkups, and paying attention to physical changes are smart ways to support long-term health.
But early awareness starts with knowing the most common signs.
Common Cervical Cancer Warning Signs You Should Not Ignore
Many of the most frequent symptoms can seem similar to routine menstrual changes or everyday gynecological issues. Still, experts from the American Cancer Society advise taking them seriously rather than waiting for them to get worse.
Watch for these common warning signs:
- Vaginal bleeding after sex, even if it is only light spotting
- Bleeding between periods
- Bleeding after menopause
- Menstrual periods that suddenly become heavier than normal
- Periods that last much longer than usual
- Watery or bloody vaginal discharge with a strong or unpleasant odor
These symptoms can feel unsettling, but they may be your body’s way of signaling that something needs attention. Research consistently shows that abnormal bleeding is one of the leading warning signs linked to cervical cancer. Keeping track of your cycle and noticing any unusual patterns can help you respond more quickly.
There are also other symptoms that many women do not immediately connect to cervical cancer.
Lesser-Known Symptoms That Are Often Missed
Bleeding and discharge usually receive the most attention, but they are not the only possible signs. Some symptoms appear gradually and may seem unrelated at first. The Mayo Clinic notes that pelvic discomfort or pain during intercourse is sometimes blamed on fatigue, endometriosis, or other common conditions. However, if these problems continue, they should be discussed with a healthcare provider.
Other possible symptoms include:
- Ongoing pelvic pain or pressure that does not improve with rest or basic pain relief
- Pain during or shortly after sexual intercourse
- Lower back pain without a clear explanation
- Swelling in the legs in more advanced cases
- Persistent tiredness
- Feeling full quickly after eating only a small amount
On their own, these symptoms may not seem urgent. But when several appear together, they can create a more complete picture. Cancer health organizations have noted that women who report multiple symptoms are often evaluated sooner, which can support better outcomes.
And then there is one symptom that many women never expect.
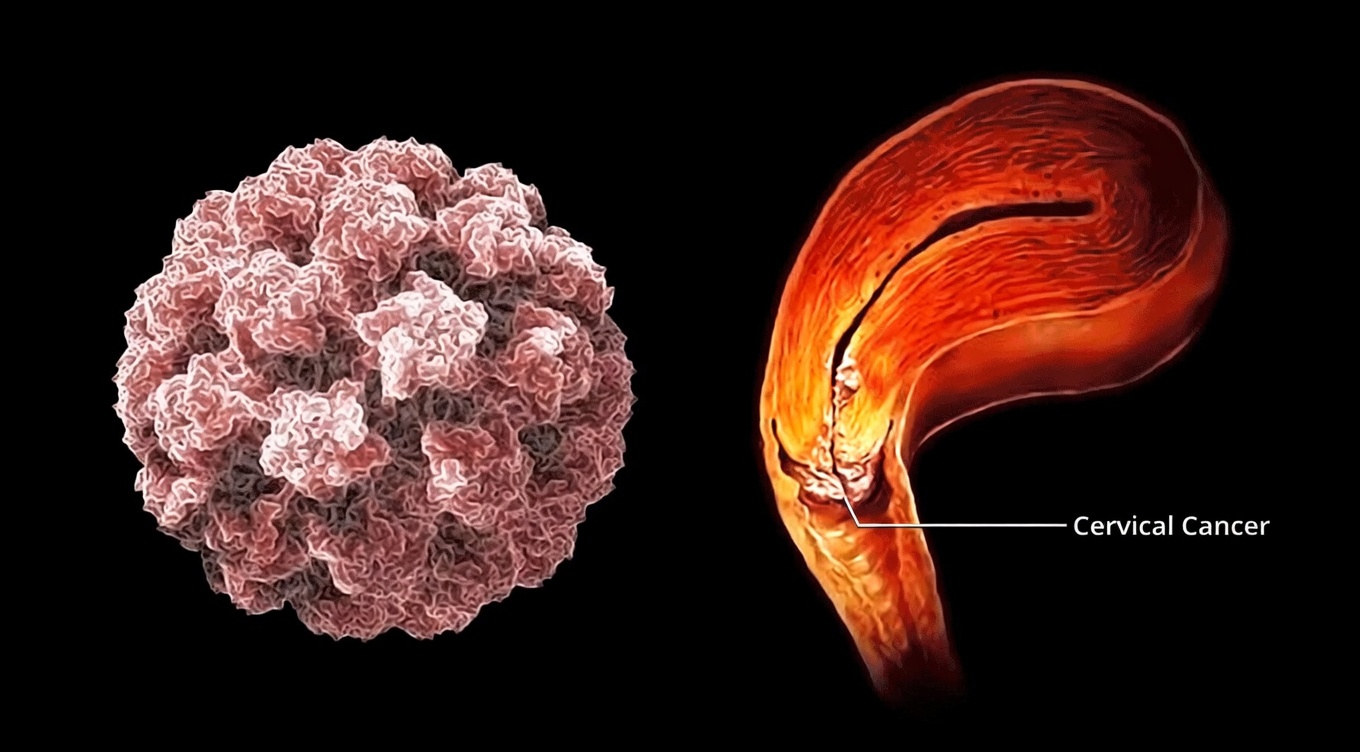
The Unexpected Symptom That Often Catches Women Off Guard
One of the most overlooked signs is a sudden change in vaginal discharge, especially when there is no bleeding at all. A difference in texture, consistency, or odor may seem minor and easy to dismiss as a yeast infection or a hormonal shift.
Yet experts warn that this kind of change can sometimes be an early sign of concern, particularly when it appears alongside other symptoms. Because it does not always seem dramatic, many women ignore it. That is exactly why it deserves more attention. Even subtle changes can matter.
Simple Steps You Can Take Right Now
Awareness is important, but action is what helps you stay in control. If something feels unusual, these practical steps can help you respond with confidence:
-
Track your symptoms
- Use your phone or a notebook for at least two weeks.
- Record dates, bleeding patterns, discharge changes, and pain levels.
-
Book an appointment with your gynecologist
- Even mild symptoms are worth checking.
- A doctor can perform tests to rule out serious concerns or identify the cause.
-
Ask about cervical cancer screening
- During your annual exam, discuss Pap tests and HPV testing.
- Screening guidelines generally begin at age 21.
-
Share your full medical history
- Mention past infections, previous abnormal test results, and any family health patterns.
- This gives your doctor a clearer overall picture.
-
Follow through on recommended follow-ups
- If anything unusual is found, ongoing monitoring is essential.
- Regular follow-up can provide both clarity and peace of mind.
These habits take very little time, but they can help you feel more informed and less anxious. Studies on health behavior show that women who monitor symptoms and seek timely care often feel more empowered in managing their health.
Why Regular Screenings Are So Important
Screening remains one of the most effective tools for staying ahead of cervical cancer. Pap tests and HPV testing can identify abnormal cell changes before symptoms even begin. The American Cancer Society emphasizes that regular screening has helped reduce cervical cancer rates significantly over the years.
Think of screening as an early alert system working in the background. By making it part of your routine healthcare, you improve your chances of catching problems early rather than relying only on symptoms to signal that something is wrong.
Still, even with consistent screenings, it is important to stay aware of your body and notice any unusual changes.
Key Takeaways Every Woman Should Remember
Cervical cancer symptoms are not always obvious, but they should never be dismissed. Changes in bleeding, discharge, pelvic pain, or energy levels may be subtle, yet they can still carry important information.
The presence of these symptoms does not automatically mean cervical cancer. In many cases, they may be caused by infections, hormonal changes, or other treatable conditions. But they are still worth discussing with a healthcare professional. When you combine symptom awareness with regular screenings, you create a strong and practical approach to protecting your health for the future.
Frequently Asked Questions
Can cervical cancer symptoms appear suddenly, or do they develop slowly?
In many cases, symptoms develop gradually. Early-stage cervical cancer may not cause any noticeable signs at all. Some women begin to notice changes over several weeks or months, which is why paying attention to your body and tracking symptoms can be so helpful.
Are these symptoms specific to cervical cancer?
No. Symptoms such as unusual bleeding, discharge, or pelvic pain can also be caused by infections, hormonal changes, or other gynecological conditions. Only a healthcare provider can determine the actual cause, so a professional evaluation is always the safest next step.
How often should screening be done if I feel healthy?
General guidelines recommend:
- A Pap test every 3 years for women ages 21 to 29
- Pap and HPV co-testing every 5 years after age 30
However, your doctor may suggest a different schedule depending on your personal medical history and risk factors.