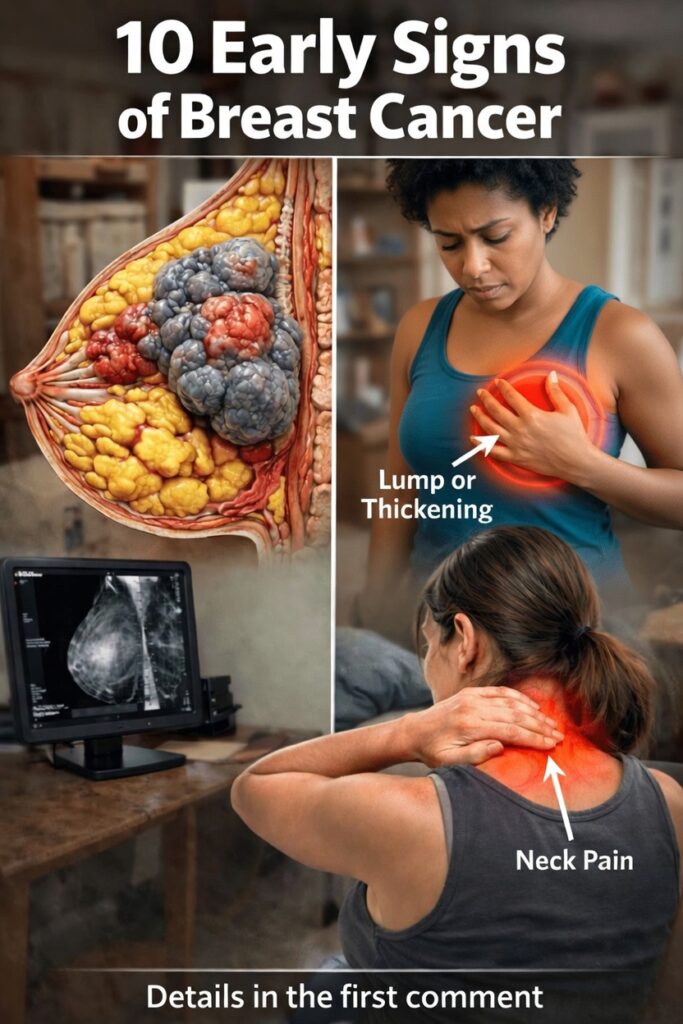
Breast Changes: Early Signs You Shouldn’t Ignore
Many women—and men—notice small changes in their breasts and quickly dismiss them as normal hormone fluctuations, mild irritation, or stress. In a busy life, these differences can seem too minor to matter. Yet putting off a checkup can sometimes give otherwise treatable conditions time to progress quietly.
The encouraging news: staying alert to what’s normal for your body and acting quickly when something seems off often leads to earlier detection, more treatment options, and better outcomes. This guide explains the key breast changes to watch for and simple ways to stay proactive. At the end, you’ll find an easy daily habit that can help you stay tuned in to your breast health.
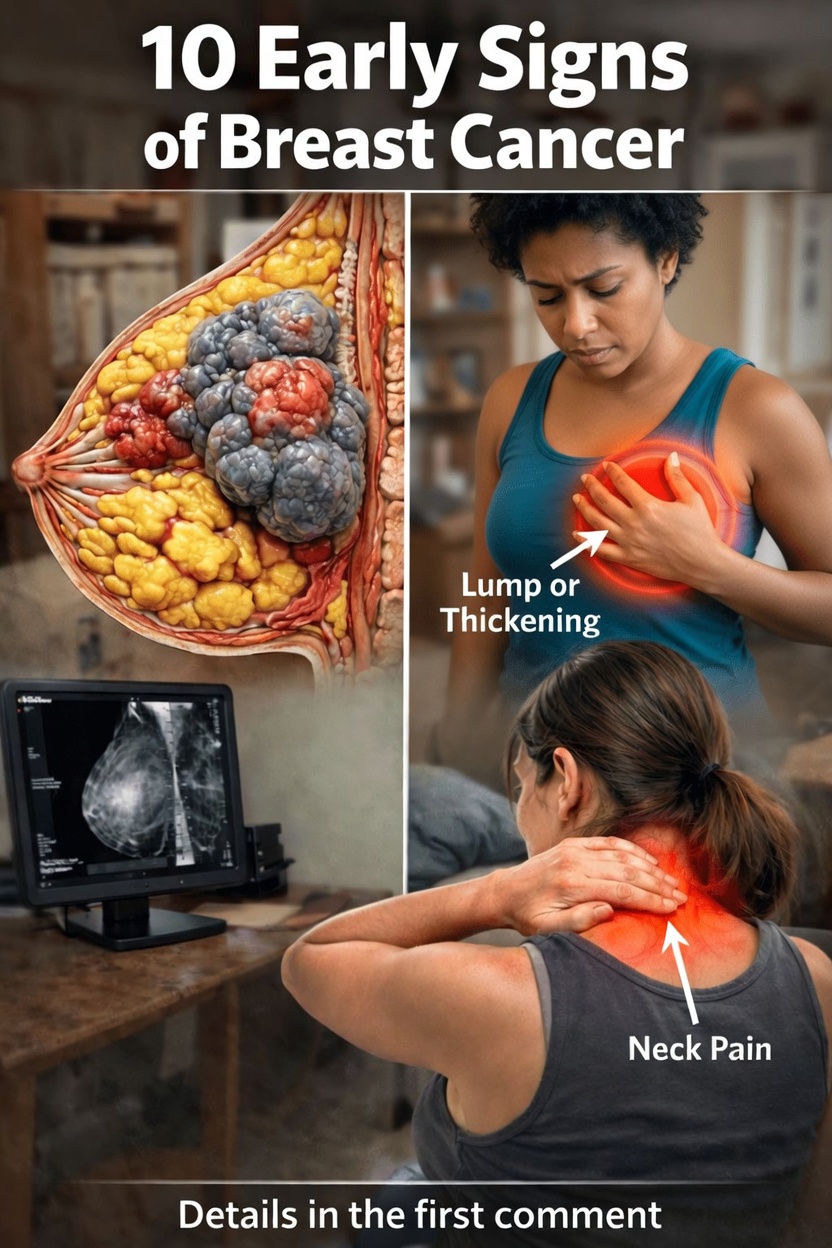
Why Paying Attention to Breast Changes Matters
Most breast cancers begin silently in the milk ducts or lobules, often without dramatic symptoms at first. According to organizations such as the American Cancer Society, when breast cancer is found early—before it has spread beyond the breast—the five‑year survival rate is around 99%. Once cancer reaches the lymph nodes or distant organs, those odds change significantly.
Hundreds of thousands of new breast cancer cases are diagnosed each year in the United States alone, yet millions of survivors are living proof that early detection works. Regular body awareness, combined with age‑appropriate screening tests, raises the chance of spotting problems at a stage when treatment is most effective.
Many people tend to “wait and see,” hoping symptoms will fade on their own. Learning what to look for shifts you from passive waiting to active, informed decision‑making.
10 Important Breast Changes You Should Not Ignore
Below are some of the most commonly reported early breast cancer signs, drawn from sources like the CDC, Mayo Clinic, and the American Cancer Society. Remember, these symptoms can also be caused by non‑cancerous conditions—but any new or persistent change should be evaluated by a healthcare professional.
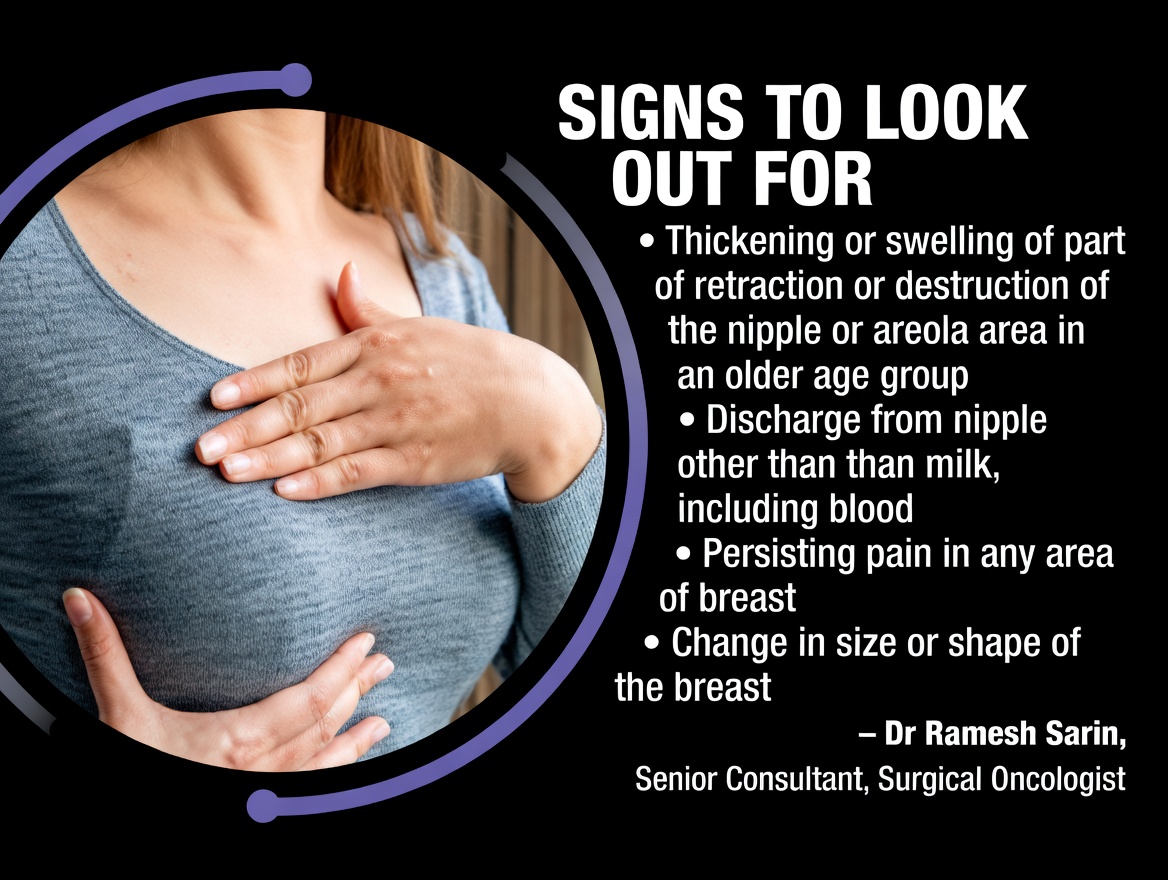
1. A New Lump or Area of Thickening
One of the most familiar warning signs is a lump or firm area that feels different from the rest of the breast tissue. Cancerous lumps often:
- Feel hard or solid
- Have irregular or uneven edges
- May not move easily under the skin
- Are usually painless
Unlike soft, fluid‑filled cysts, these areas tend to be more rigid. Any newly discovered lump—no matter how small—should prompt an appointment with your doctor.
2. Unexplained Change in Breast Size, Shape, or Contour
If one breast suddenly appears larger, smaller, higher, or lower than the other, and the change cannot be explained by your menstrual cycle, pregnancy, weight changes, or breastfeeding, it deserves attention. Make note of:
- Asymmetry that is new or more pronounced
- Changes that persist longer than two weeks
3. Skin Dimpling, Puckering, or “Orange Peel” Texture
Skin that looks dimpled, puckered, or similar to the surface of an orange (peau d’orange) can be a sign that something beneath the skin is pulling the tissue inward. To check:
- Raise your arms and observe your breasts in a mirror
- Place your hands on your hips and flex your chest muscles
If the skin does not move symmetrically or shows new dimpling or puckering, seek medical advice.
4. Redness, Warmth, or Persistent Itching
Breast skin that appears red, inflamed, warm to the touch, or constantly itchy—and does not improve with typical treatments—may indicate an inflammatory form of breast cancer. These types are less common but can progress quickly, so prompt evaluation is important.
5. Ongoing Pain in One Specific Area
Most breast pain is related to hormonal shifts and comes and goes with your cycle. However, pain that:
- Is focused in one spot
- Does not fluctuate with your period
- Persists over time
should be checked. While breast pain alone is rarely a sign of cancer, it can be associated with underlying issues that need attention.
6. Swelling in the Breast or Underarm
Unexplained swelling, heaviness, or fullness in the breast—sometimes even before a lump can be felt—can be a warning sign. Also check:
- The armpit area for enlarged or tender lymph nodes
- Any difference in breast size that feels new or unusual
7. New Nipple Inversion (Turning Inward)
Some people are born with inverted nipples, which is usually harmless. However, if a nipple that was previously outward becomes newly inverted or pulled in, it may signal a change in the underlying tissue and should be evaluated.
8. Changes in the Nipple or Areola Skin
Skin around the nipple (the areola) that becomes red, scaly, crusted, or thickened and does not improve with typical skin treatments may be a sign of an underlying condition such as Paget’s disease of the breast, a rare form of cancer. Symptoms can resemble eczema but persist despite creams or ointments.
9. Unusual Nipple Discharge
Nipple discharge that:
- Occurs spontaneously (without squeezing)
- Comes from one breast only
- Is bloody, clear, or watery
is considered more concerning and should be checked, especially if you are not breastfeeding or recently pregnant. Any new or unexplained discharge is worth discussing with your healthcare provider.
10. Swollen or Firm Lymph Nodes
Hard, enlarged, and usually painless lymph nodes under the arm or above the collarbone can sometimes indicate that breast cancer has spread. Gently feel:
- High in the armpit
- Around the collarbone
Persistent firmness or swelling in these areas should be assessed promptly.
Keep in mind: some people have more than one of these symptoms at the same time, while others have no noticeable changes early on. This is why recommended screening tests, such as mammograms, are crucial—they can detect abnormalities before they can be felt.
Simple, Practical Steps for Better Breast Awareness
These daily and monthly habits can help you stay familiar with your own “normal” and spot changes sooner.

1. Establish a Monthly Self-Check Routine
Choose a consistent date each month. For people who menstruate, the best time is usually a few days after your period ends, when breasts tend to be less tender and swollen.
Use this simple routine:
-
In front of a mirror
- Stand with arms at your sides, then raise them overhead.
- Next, place your hands on your hips and gently press to flex your chest muscles.
- In each position, look for changes in size, shape, skin texture, or nipple appearance.
-
Lying down
- Lie on your back with a pillow under your shoulder on the side you are checking.
- Use the opposite hand to feel the breast with the pads of your fingers in small circular motions.
- Cover the entire breast and armpit area, moving from the collarbone down to the bra line and from the center of the chest out to the side.
-
Nipple check
- Gently squeeze each nipple and check for any discharge or pain.
Document what you notice using notes or photos taken in similar lighting and positions each month. This makes subtle changes easier to spot.
2. Track Changes Over Time
Use a notebook, calendar, or health app to log:
- Any new lumps, pain, or skin changes
- When they started
- Whether they change with your cycle
Anything that lasts longer than about two weeks or feels different from your usual pattern should be reviewed by a healthcare professional.
3. Stay Up to Date with Recommended Screenings
Screening guidelines can vary by country and health organization, but many recommend:
- Starting routine screening mammograms around age 40 for people at average risk
- Considering earlier and/or more frequent screening if you have a strong family history, genetic mutations (such as BRCA1/2), prior chest radiation, or other risk factors
Discuss your personal and family history with your provider so you can create a screening schedule tailored to your risk level.
4. Know Your Risk Factors
Certain factors increase the likelihood of developing breast cancer, including:
- Increasing age
- Family history of breast or ovarian cancer
- Dense breast tissue
- Specific genetic mutations (e.g., BRCA1, BRCA2)
- Certain hormonal or reproductive histories
Knowing your risk does not mean cancer is inevitable—it simply helps you and your doctor choose the most appropriate screening and prevention strategies.
Quick Guide: Common vs. Concerning Breast Changes
Use this comparison to help distinguish between changes that are often harmless and those that should be checked promptly. This is not a substitute for medical advice, but it can guide your next step.
Changes That Are Often Benign
- Tenderness that comes and goes with your menstrual cycle
- Soft, movable lumps that change in size with your cycle
- Nipple discharge only during breastfeeding or shortly after weaning
- Mild, temporary swelling before your period
Changes That Need Prompt Medical Review
- A hard, fixed lump that does not move easily under the skin
- Spontaneous bloody or clear nipple discharge, especially from one breast
- New skin dimpling, thickening, or redness that does not resolve
- A newly inverted nipple or persistent, localized breast pain
If you are ever unsure which category your symptom fits into, it is safer to ask a healthcare professional.
When to Contact a Healthcare Provider Immediately
Seek medical attention as soon as possible if you notice:
- Rapid onset of breast redness, swelling, and warmth
- Bloody nipple discharge accompanied by a lump
- A firm, fixed breast lump along with swollen lymph nodes in the armpit or near the collarbone
Quick evaluation can offer reassurance when everything is normal—or catch serious problems at a more treatable stage.
Wrapping Up: Small Daily Actions, Lasting Protection
Paying close attention to breast changes is a powerful form of self‑care. By combining:
- Monthly self‑checks
- Consistent tracking of changes
- Regular mammograms and clinical exams
you give yourself the best chance of detecting problems early. Share this information with family and friends so they, too, can be more aware. Early recognition and prompt evaluation truly can change outcomes.
Frequently Asked Questions
When should screening mammograms start?
Many guidelines recommend starting routine screening mammograms around age 40 for people at average risk, with exams every one to two years. Individuals at higher risk—because of strong family history, genetic mutations, or other factors—may need to begin earlier and screen more often. Talk with your doctor about the right plan for you.
Can men have breast cancer or breast cancer symptoms?
Yes. While male breast cancer is rare, it does occur. Because men have less breast tissue, they may notice:
- Lumps under or near the nipple
- Nipple discharge
- Nipple or skin changes
- Swelling near the breast or underarm
The warning signs are similar to those in women, and early evaluation is equally important.
Do these breast changes always mean cancer?
No. Most breast changes turn out to be benign conditions such as cysts, fibroadenomas, or hormonal fluctuations. However, only a medical professional can determine the cause through physical exams, imaging (like mammograms or ultrasounds), and sometimes biopsies. Awareness is meant to prompt timely evaluation—not panic.
Medical Disclaimer
This article is for general information only and does not replace professional medical advice, diagnosis, or treatment. If you notice any breast changes or have concerns about your breast health, consult a qualified healthcare provider. Regular screenings and professional evaluations remain essential for early detection and effective care.