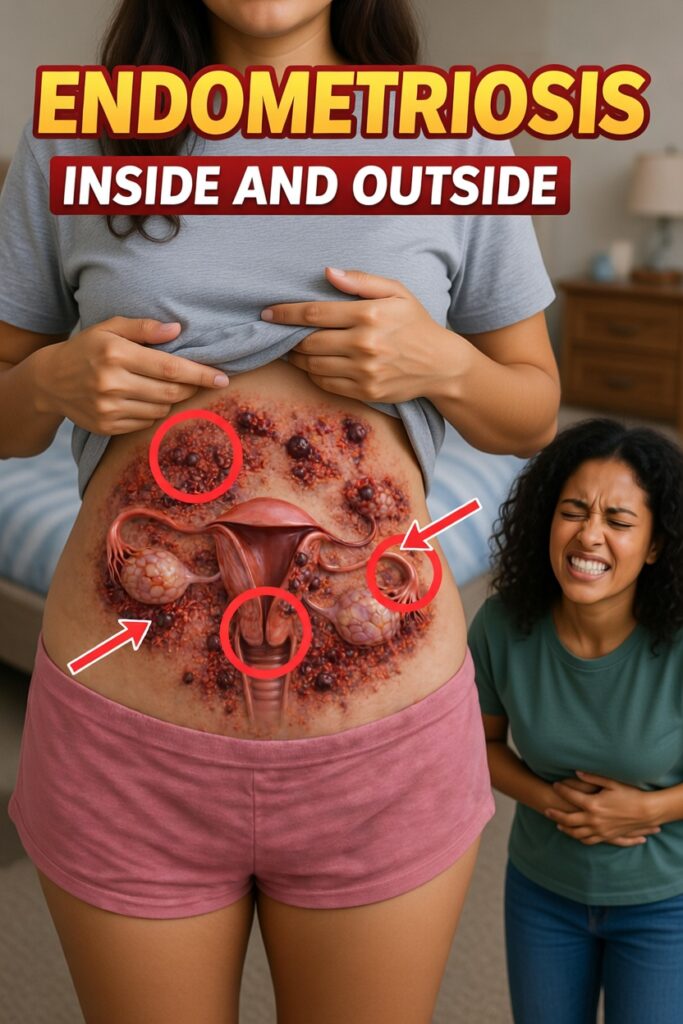
Living With Endometriosis: Why Your Pain Is Not “Just Cramps”
For many women, period pain is far more than a monthly inconvenience. Intense pelvic pain can interrupt work, strain relationships, and make everyday activities feel overwhelming. For some, the discomfort is not limited to menstruation—it lingers throughout the month and may come with extreme fatigue, heavy bleeding, or difficulty getting pregnant. The search for answers can feel lonely and exhausting.
Endometriosis affects millions of women around the world, yet it is still underrecognized and frequently dismissed as “normal period pain.” Understanding the condition and adopting supportive lifestyle strategies can make daily life more manageable. Below you’ll find practical steps many women use to navigate endometriosis more comfortably.
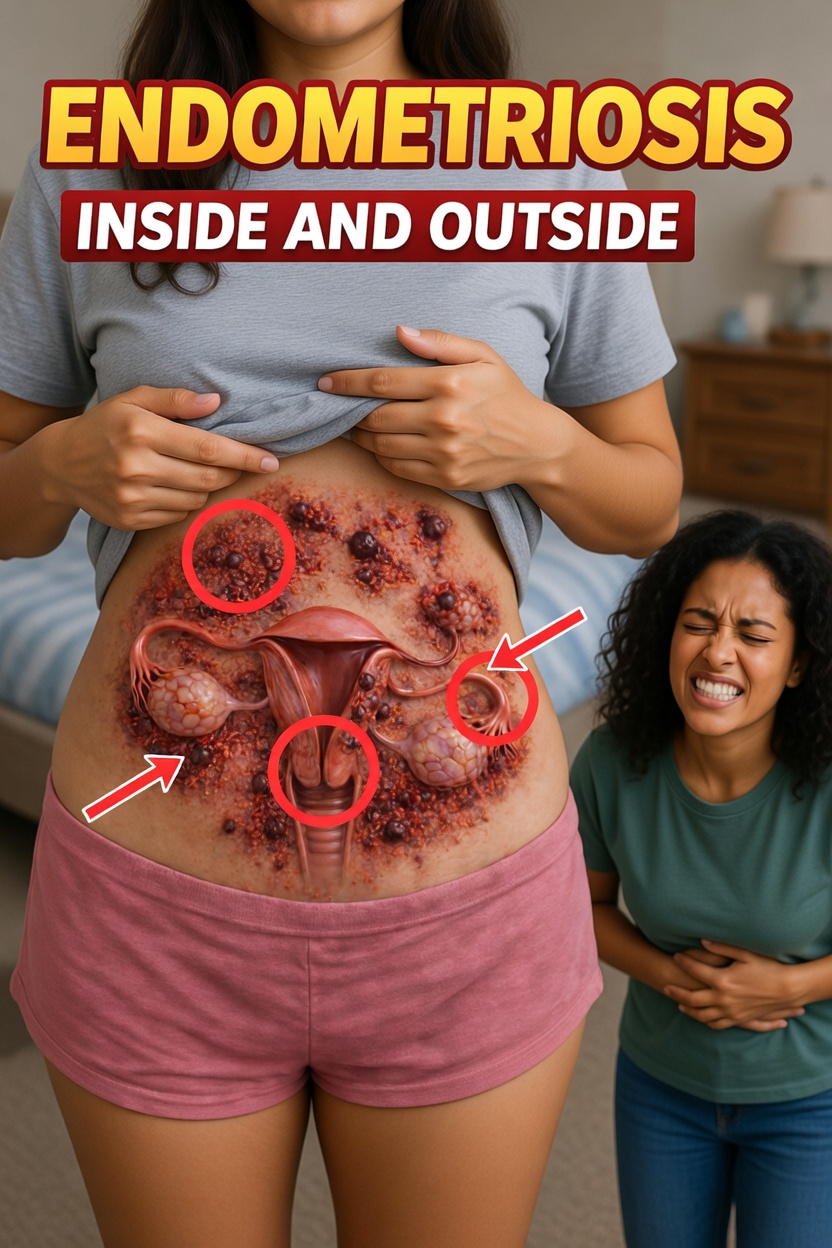
What Exactly Is Endometriosis?
Endometriosis is a chronic condition in which tissue similar to the lining of the uterus (the endometrium) grows outside the uterus. These endometrial-like cells can appear on the:
- Ovaries
- Fallopian tubes
- Pelvic walls and lining
- Occasionally, other nearby organs
Just like the uterine lining, this tissue responds to hormonal changes during the menstrual cycle. It thickens, breaks down, and bleeds each month. However, because it is located outside the uterus, the blood and tissue have no natural way to leave the body. Over time, this can cause:
- Inflammation
- Scar tissue (fibrosis)
- Adhesions, where organs stick to each other
According to data from organizations such as the World Health Organization, endometriosis affects roughly 10% of women of reproductive age globally—around 190 million people. It is most commonly diagnosed in women in their 20s to 40s, though it can appear earlier in adolescence or later in adulthood.
Possible Causes of Endometriosis
The precise cause of endometriosis is still unknown, but several theories help explain why it develops in some women and not others:
- Retrograde menstruation: Menstrual blood flows backward through the fallopian tubes into the pelvic cavity instead of leaving the body, carrying endometrial-like cells with it.
- Immune system differences: An altered immune response may fail to identify and remove these misplaced cells, allowing them to implant and grow.
- Genetic factors: Endometriosis often runs in families, suggesting a hereditary component.
- Hormonal and environmental influences: Hormone levels and certain environmental exposures may contribute to abnormal tissue growth.
None of these explanations fully accounts for every case, but together they provide insight into how and why endometriosis may develop.
Common Signs and Symptoms of Endometriosis
Endometriosis looks different for everyone. Some women have mild discomfort, while others experience severe, life-altering symptoms. Typical signs include:
- Pelvic pain that intensifies around menstruation and may be present at other times in the cycle
- Severe menstrual cramps (dysmenorrhea) that make daily tasks or work difficult
- Pain during or after sex (dyspareunia)
- Painful bowel movements or urination, particularly during periods
- Heavy, prolonged, or irregular menstrual bleeding
- Fatigue, bloating, nausea, or digestive issues around menstruation
- Trouble conceiving, in some women
Research from institutions such as the Mayo Clinic and Cleveland Clinic notes that pain often peaks just before and during menstruation, driven by cyclical hormone changes and inflammation. Many women describe the pain as exhausting and debilitating, interfering with:
- Sleep
- Concentration
- Mood
- Overall quality of life
Emotional and Mental Health Impact
Endometriosis affects more than the body. Ongoing pain, delays in diagnosis, and feeling dismissed or misunderstood can lead to:
- Frustration and anger
- Anxiety and low mood
- Feelings of isolation
Recognizing this emotional burden is important—both physical and mental health deserve attention and care.
How Endometriosis Is Diagnosed
Endometriosis can be challenging to identify because its symptoms overlap with other conditions, such as irritable bowel syndrome (IBS) or pelvic inflammatory disease.
A typical diagnostic process may include:
-
Detailed medical history and symptom review
Your healthcare provider will ask about your pain, menstrual cycle, fertility concerns, and family history. -
Pelvic exam
A physical exam can sometimes detect cysts or areas of tenderness suggestive of endometriosis. -
Imaging tests
Ultrasound or MRI may help visualize ovarian cysts or other abnormalities, though they do not always show all endometriosis lesions. -
Laparoscopy
In many cases, a minimally invasive surgery called laparoscopy is used to confirm the diagnosis. A small camera is inserted through a tiny incision to look for endometriosis tissue and, in some cases, remove or biopsy it.
Because symptoms can mimic other problems, it often takes years for women to receive a clear diagnosis. Speaking with a healthcare professional early and persistently is crucial if your pain feels severe or “not normal” for you.

Everyday Strategies to Help Manage Endometriosis Symptoms
There is currently no cure for endometriosis, but many women find that consistent, supportive habits can reduce symptom intensity and improve daily comfort. Consider the following approaches and adapt them to your needs:
1. Track Your Cycle and Symptoms
- Use a period-tracking app or a simple notebook.
- Record pain levels, location of pain, mood changes, digestive issues, and bleeding patterns.
- Note what seems to worsen or ease symptoms (foods, activities, stress).
This information can help you anticipate flare-ups and provide valuable insight for your healthcare provider.
2. Incorporate Gentle Movement
Regular, low-impact exercise can improve circulation, reduce stiffness, and support mental health without overloading the body. Helpful options include:
- Walking
- Swimming or water aerobics
- Gentle yoga or stretching routines
Aim for consistency rather than intensity, adjusting based on how you feel each day.
3. Focus on an Anti-Inflammatory Eating Pattern
Diet alone will not eliminate endometriosis, but many women report feeling better with an anti-inflammatory approach:
- Emphasize whole, unprocessed foods.
- Include omega-3-rich options like salmon, sardines, walnuts, and flaxseeds.
- Eat plenty of colorful fruits and vegetables.
- Choose whole grains over refined grains.
- Limit highly processed foods, sugary drinks, and excessive alcohol.
If possible, consult a dietitian familiar with endometriosis or women’s health for personalized guidance.
4. Use Heat for Pain Relief
Heat can relax muscles and increase blood flow, providing quick relief for pelvic pain:
- Apply a heating pad or hot water bottle to the lower abdomen or lower back.
- Take a warm bath or shower during flare-ups.
Always follow safety instructions to avoid burns.
5. Practice Stress-Reduction Techniques
Stress can make pain feel more intense. Simple mind–body practices may help calm the nervous system:
- Deep breathing exercises
- Guided meditation or mindfulness apps
- Gentle progressive muscle relaxation
- Short, regular breaks during the day to reset
Even 5–10 minutes of intentional relaxation can be beneficial.
6. Protect Your Sleep and Rest
Fatigue can heighten the perception of pain, so prioritizing rest is vital:
- Aim for a regular sleep schedule.
- Create a calming bedtime routine (dim lights, no screens, relaxation techniques).
- Allow yourself extra rest during particularly painful days, if possible.
Quick Symptom-Relief Tips (At-a-Glance)
For faster reference during flare-ups:
- Take over-the-counter anti-inflammatory medications (such as ibuprofen) at the start of your period, following dosage directions and medical advice.
- Drink plenty of water and reduce caffeine and salty foods around your period to help ease bloating.
- Wear soft, loose-fitting clothing to avoid pressure on your abdomen and pelvis.
- Ask a pelvic floor physical therapist or specialist about relaxation and stretching exercises tailored to pelvic pain.
- Join support groups—in person or online—to connect with others who understand what you are going through.
Studies suggest that combining lifestyle modifications with medical care often leads to the best improvements in comfort and function.
When to Seek Professional Help
It is important to reach out to a healthcare provider if:
- Pelvic pain regularly interferes with your work, school, or daily activities.
- Your periods are becoming heavier, longer, or more painful over time.
- You have been trying to conceive without success and suspect endometriosis may be involved.
- Pain relief methods at home are no longer effective.
A gynecologist or endometriosis specialist can discuss options such as:
- Hormonal treatments (e.g., birth control pills, hormonal IUDs, or other hormone therapies)
- Pain management plans
- Surgical options in selected cases
- Multidisciplinary care, including pain specialists, physical therapists, and mental health professionals
Individualized treatment—built around your unique symptoms and goals—is key.
Key Takeaways
- Endometriosis is a long-term condition in which tissue similar to the uterine lining grows outside the uterus, affecting millions worldwide.
- Common symptoms include pelvic pain, heavy or irregular periods, pain with sex, digestive issues, fatigue, and sometimes infertility.
- The exact cause is not fully understood, but genetic, hormonal, immune, and environmental factors are thought to play a role.
- Early recognition and diagnosis can help, but many women face delays, so persistent advocacy for your health is important.
- Lifestyle changes—such as tracking symptoms, gentle movement, anti-inflammatory eating, stress reduction, and good sleep—can support medical treatment and improve day-to-day comfort.
You are not alone, and your pain is real. With knowledge, support, and the right care, many women with endometriosis are able to regain a greater sense of control over their bodies and their lives.
Frequently Asked Questions (FAQ)
What is the main symptom of endometriosis?
The hallmark symptom is pelvic pain, often more intense than typical menstrual cramps. This pain usually worsens before and during periods but may also occur at other times in the cycle.
Can endometriosis affect fertility?
Yes. Endometriosis can contribute to difficulty getting pregnant due to inflammation, scarring, and adhesions that may interfere with the reproductive organs. However, many women with endometriosis do conceive—either naturally or with fertility support.
Is endometriosis the same as normal period pain?
No. While some period discomfort can be normal, endometriosis pain is often more severe, longer lasting, and may come with additional symptoms such as heavy bleeding, pain with sex, bowel or bladder discomfort, and chronic fatigue. If your pain feels excessive or disruptive, it is important to seek medical advice.