Subtle Facial Changes After Sleep: What They May Reveal About Brain Health
Many people go to bed feeling perfectly fine, then notice something unusual the next morning while looking in the mirror. One of the most easily missed changes is mild facial unevenness or a slight droop on one side, especially after sleeping. It can be unsettling, and for good reason, because sudden facial changes may raise concerns about serious neurological issues.
The reassuring news is that understanding these overnight signs and building a few simple daily habits can help you recognize body changes earlier and respond appropriately.
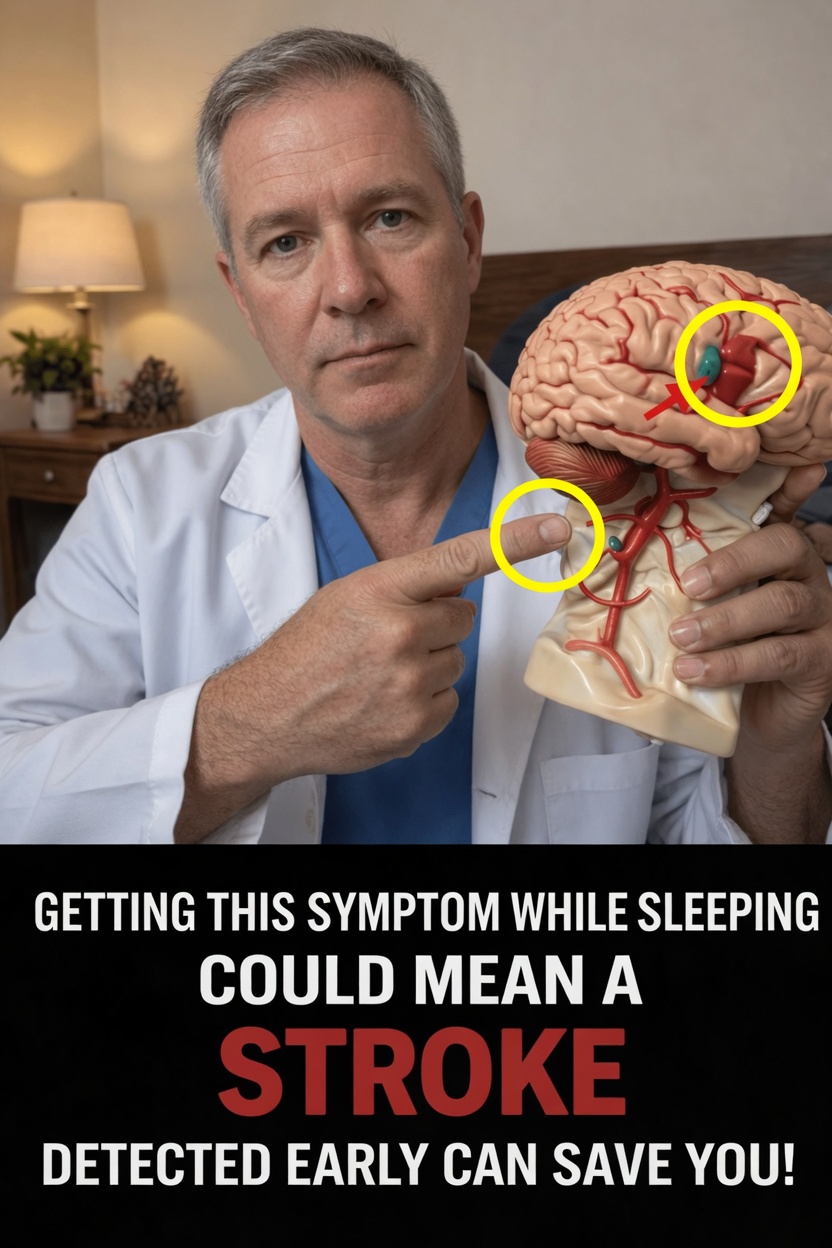
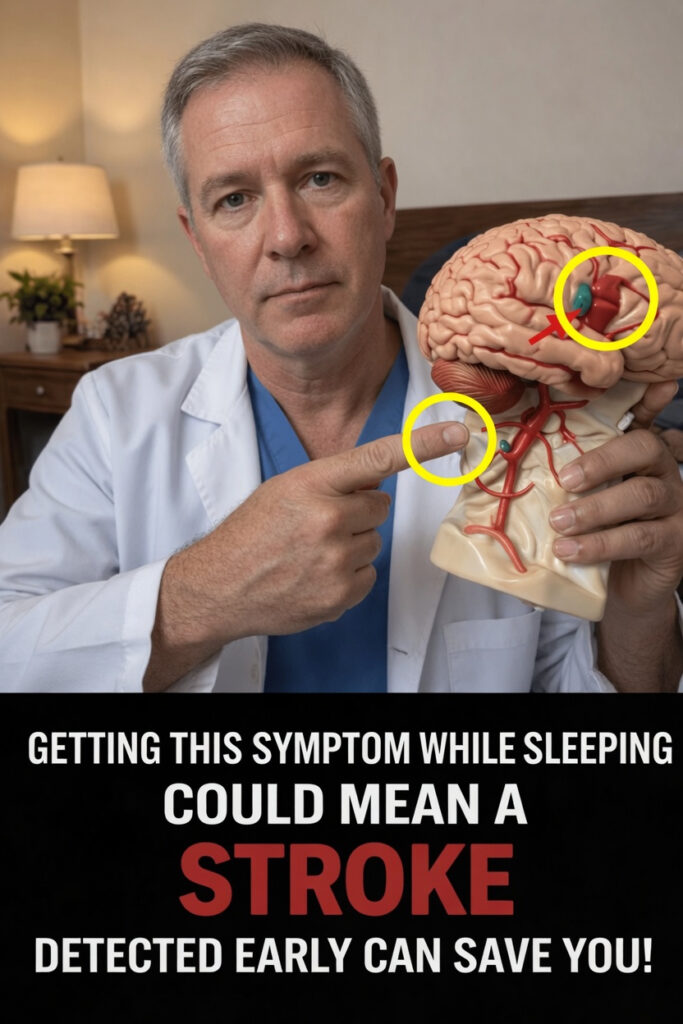
The image associated with this topic shows a healthcare professional holding a brain model, with a red arrow highlighting one area. It visually emphasizes an important point: signs that appear during rest or after waking may sometimes be connected to major brain events such as stroke. No single symptom can predict exactly what will happen, but noticing repeated patterns during sleep or first thing in the morning can support earlier medical attention and better conversations with your doctor.
Overnight Symptoms and Their Link to Stroke Risk
A stroke can happen at any hour, including while a person is asleep. That is why some individuals first become aware of symptoms only after they wake up. Medical research shows that a significant share of strokes occur overnight. These are often referred to as wake-up strokes, because warning signs become noticeable in the morning.
Common symptoms may include:
- Sudden facial drooping
- Weakness on one side of the body
- Slurred or altered speech
Online claims sometimes suggest that a specific sign appears exactly three days before a stroke during sleep. However, trusted medical sources do not support a fixed countdown like that. In most cases, stroke symptoms begin suddenly. That said, some people experience brief episodes beforehand known as transient ischemic attacks (TIAs). These temporary events may happen days or even weeks before a more serious stroke.
Although TIAs often pass quickly, they should never be ignored. They may indicate that blood flow to the brain has been briefly reduced or blocked.
Organizations such as the American Heart Association and Mayo Clinic also note that obstructive sleep apnea (OSA) is linked to a higher stroke risk. Repeated pauses in breathing during sleep can affect:
- Oxygen levels
- Blood pressure
- Blood vessel health
- Overall cardiovascular function
Because of this, recurring nighttime symptoms deserve attention.
Facial Drooping After Sleep: A Sign Worth Noticing
One of the most talked-about warning signs is facial drooping or asymmetry that becomes obvious after waking. For stroke awareness, health experts widely use the FAST method:
- Face drooping – Does one side of the face appear lower when smiling?
- Arm weakness – Does one arm drift downward when both arms are raised?
- Speech difficulty – Is speech slurred, unclear, or unusual?
- Time to call emergency services – Immediate action is critical
If you or someone close to you notices that one side of your face looks different in the morning, such as a drooping eyelid, uneven smile, or lowered corner of the mouth, do not dismiss it. In some cases, this may reflect how the brain is controlling facial muscles.
Still, stroke is not the only possible explanation. Facial asymmetry can also happen because of:
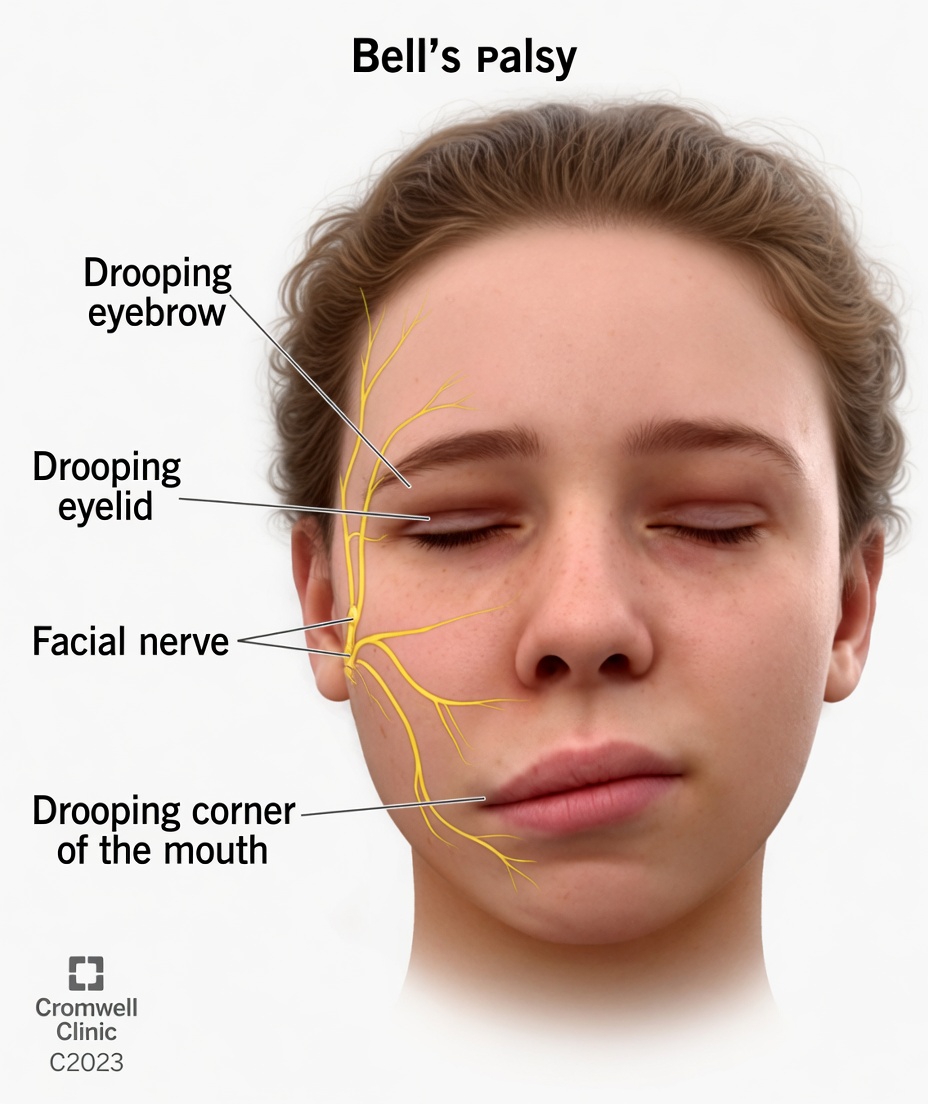
- Bell’s palsy
- Fatigue
- Allergies or swelling
- Pressure from sleeping position
This is why proper medical evaluation matters.
Morning Signs to Watch For
Pay close attention to symptoms such as:
- A sudden crooked smile or one-sided facial droop upon waking
- Brief numbness or tingling on one side of the face
- Symptoms that improve later in the day but keep coming back
- Dizziness, brain fog, or mild confusion in the morning
These changes do not automatically mean a stroke has occurred, but they should not be brushed aside, especially if they are new, sudden, or repeated.
Daily Habits That Support Brain and Sleep Health
No lifestyle change can promise complete prevention, but research consistently links certain habits with lower vascular risk. Many health professionals recommend the following steps:
- Keep a regular sleep schedule
- Maintain healthy blood pressure through diet and exercise
- Get medical help for sleep apnea or suspected breathing problems during sleep
- Stay active most days of the week
- Eat a balanced diet with fruits, vegetables, whole grains, and healthy fats
- Avoid smoking
- Limit alcohol intake
- Drink enough water
- Check cholesterol and blood sugar regularly
These actions support both brain health and overall circulation.
Simple Steps You Can Start Tonight
A few practical habits can improve awareness of your sleep patterns and physical changes:
- Look at your face in the mirror each morning. Smile and check whether both sides move evenly.
- Lightly touch both sides of your face to notice numbness or unusual sensation.
- Ask a partner or family member whether you snore loudly, stop breathing briefly, or seem unusually restless at night.
- Keep a short sleep journal for one week, recording facial changes, morning energy, and any odd sensations.
- Follow good sleep hygiene by keeping the room cool and dark, sleeping at a consistent time, and reducing screen use before bed.
- Schedule regular medical check-ups to review blood pressure, sleep quality, and other vascular risk factors.
These small routines can help you understand what is normal for your body, making unusual changes easier to spot.
Why Sleep Position and Breathing Deserve Attention
Sleeping on the back can worsen snoring or breathing interruptions in some people, especially those prone to sleep apnea. For certain individuals, side sleeping with good pillow support may be more comfortable and may reduce nighttime breathing problems.
Untreated sleep-disordered breathing has been associated with:
- Higher blood pressure
- Greater cardiovascular strain
- Increased stroke risk over time
If you suspect breathing issues during sleep, speak with a doctor about screening. A sleep study may help identify the problem, and treatment options such as CPAP therapy may be recommended when appropriate.
Inflammation and blood vessel health also play an important role. Chronic conditions that damage circulation can affect how well the brain receives blood flow, including during sleep when the body is recovering.
Normal Morning Changes vs. Possible Warning Signs
It can help to compare common sleep-related experiences:
- Usually normal: Mild morning puffiness caused by fluid shifts during sleep that improves soon after getting up
- Potential concern: One-sided facial drooping or weakness that lasts beyond a few minutes, especially with speech or arm changes
- Other possible cause: Temporary numbness from pressure on a nerve due to sleeping posture, which often improves after moving
When a change is sudden, unusual, or persistent, it is safest to treat it seriously.
Long-Term Habits for Better Awareness
Beyond checking symptoms day to day, these habits can support long-term health monitoring:
- Take gentle evening walks to support circulation and sleep quality
- Use relaxation methods before bed, such as deep breathing or light stretching
- Keep up with yearly health screenings for blood pressure, cholesterol, and diabetes
- If you have known risk factors like hypertension, diabetes, or family history, ask your doctor about personalized monitoring
Tracking these areas can make medical visits more productive and help you identify patterns sooner.
What to Do If You Notice Something Unusual
If you wake up with facial drooping along with any of the following, seek emergency medical care immediately:
- Arm or leg weakness
- Trouble speaking
- Vision changes
- Severe headache
- Loss of balance or coordination
Time is extremely important in these situations. Fast treatment can greatly affect recovery and outcomes. Even if symptoms disappear quickly, they still need medical attention because they may represent a TIA or another serious condition.
Frequently Asked Questions
Do facial changes after sleep always mean something serious?
No. Temporary asymmetry can happen because of sleeping position, allergies, swelling, or minor nerve pressure. However, if the change is sudden, clearly one-sided, or appears with other symptoms, it should be evaluated by a medical professional.
How common are strokes during sleep?
Strokes that occur during sleep are well recognized and are often called wake-up strokes because symptoms are first noticed in the morning. They are not rare, which is why unusual signs upon waking should be taken seriously.
Can sleep apnea raise stroke risk?
Yes. Obstructive sleep apnea is associated with higher stroke and cardiovascular risk. Repeated breathing interruptions can lower oxygen levels and place added stress on the heart and blood vessels.
Should temporary symptoms still be reported?
Absolutely. Even if facial numbness, drooping, or weakness improves quickly, it may still signal a transient ischemic attack. A prompt medical assessment is important.
Final Takeaway
A slightly uneven face after sleep may be harmless, but it can also be an early clue that something more serious needs attention. Because strokes can happen overnight, symptoms first noticed in the morning should never be ignored. Watching for recurring facial changes, breathing disturbances, and other neurological symptoms can help you respond faster and protect long-term brain health.
The key message is simple: stay observant, build healthy sleep and lifestyle habits, and seek medical help quickly when symptoms appear suddenly.