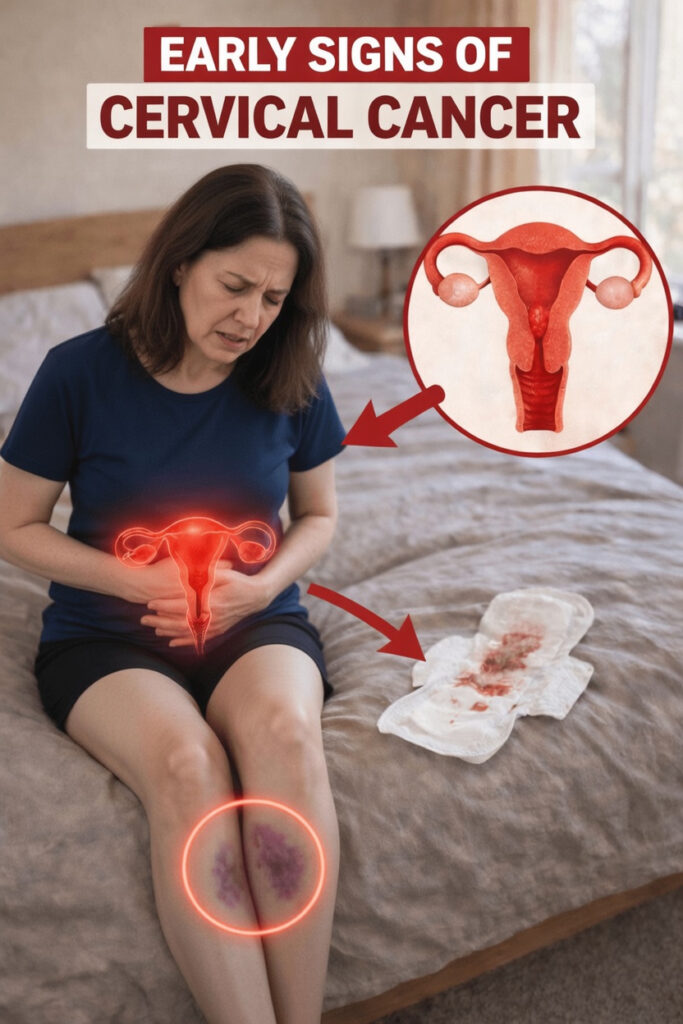
9 Early Signs of Cervical Health Problems Women Should Not Ignore
Many women notice small physical changes and assume they are caused by stress, hormonal fluctuations, or minor day-to-day discomfort. At first, these signals may seem too mild to matter. But when they continue or become more noticeable, they should not be overlooked.
Being aware of recurring symptoms and knowing when to consult a healthcare professional can help you take a more proactive approach to your well-being. One important issue is that a certain symptom often appears in everyday life and is easy to dismiss until much later. Below are nine early warning signs that deserve attention, plus practical actions you can take now.
Why Early Awareness of Cervical Health Is Important
Cervical cancer usually develops gradually. In the earliest stages, it may not cause any obvious symptoms. According to leading health organizations such as the Mayo Clinic and the American Cancer Society, regular screening with Pap tests and HPV tests is essential because it can detect abnormal changes before they become more serious.
Even so, as the body changes, some women may begin to notice signs that feel unusual. These symptoms are not specific only to cervical cancer and may be linked to other conditions as well. That is exactly why medical evaluation matters. Many women postpone seeing a doctor because the symptoms seem familiar, mild, or easy to explain away, such as irregular bleeding or slight pelvic discomfort.
Once you know what to watch for, it becomes easier to recognize when something deserves a closer look.
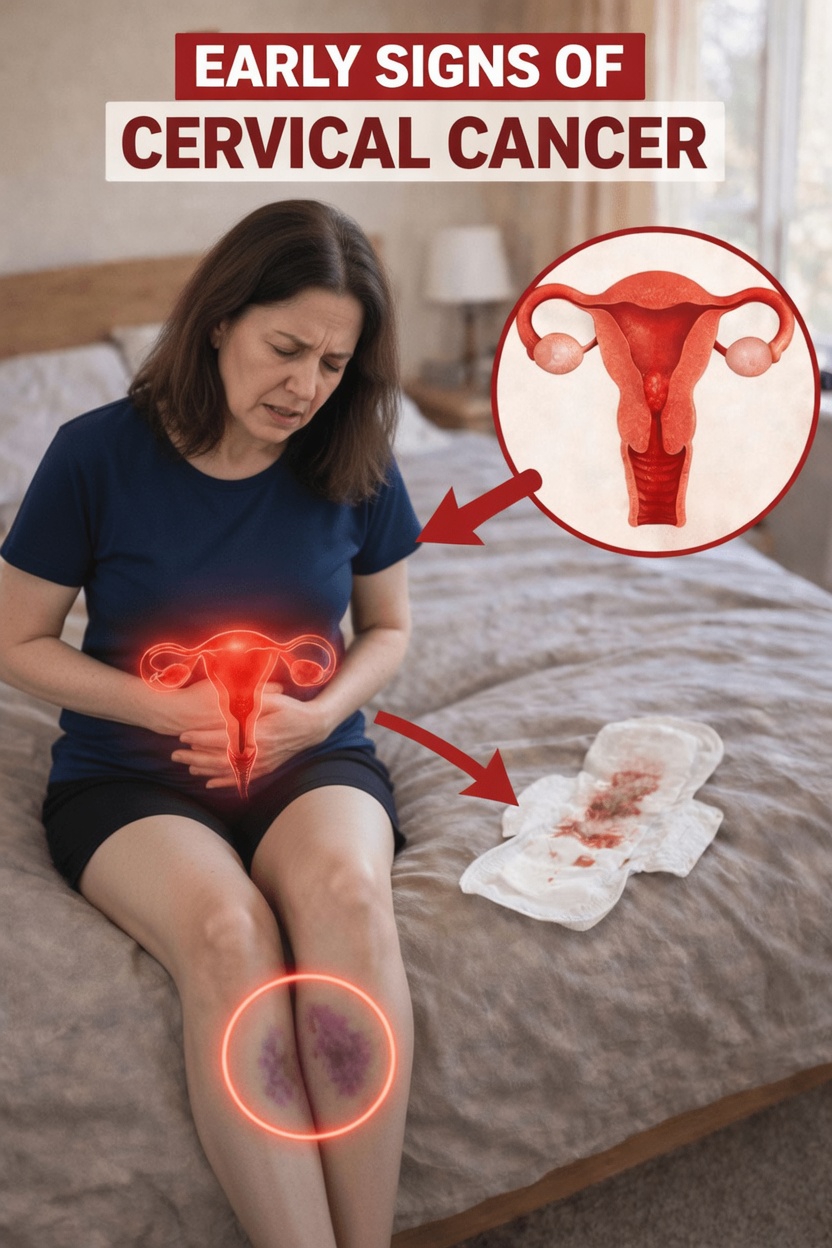
1. Unusual Vaginal Bleeding
Unexpected bleeding is one of the most commonly reported warning signs. This may include:
- Spotting between periods
- Bleeding after sex
- Bleeding after menopause
- Periods that suddenly become heavier
- Menstrual bleeding that lasts longer than usual
It is easy to blame these changes on stress or hormones. However, any bleeding pattern that is new or outside your normal cycle should be discussed with a healthcare provider.
If this has happened to you, try recording when it occurs, how much bleeding there is, and whether anything seems to trigger it. That information can be helpful during a medical appointment.
2. Changes in Vaginal Discharge
Vaginal discharge is normal, but lasting changes in color, texture, amount, or odor may need attention. Signs to watch for include discharge that is:
- Watery
- Pink, brown, or blood-streaked
- Heavier than usual
- Strong-smelling or unpleasant
Some women assume these changes are caused by diet or infection. But if the difference does not go away on its own, it is worth mentioning to your doctor. Discharge that contains blood or has a foul odor is often listed in cervical health awareness resources.
3. Pain During or After Intercourse
Discomfort during sex that is new, recurring, or worsening should not be ignored. Some women describe it as:
- A deep pelvic ache
- Sharp pain
- Lingering soreness after intercourse
Because this can sometimes be blamed on dryness, position, or temporary irritation, many people dismiss it. But if it continues or becomes more intense, it should be evaluated by a medical professional.
4. Ongoing Pelvic Pain or Pressure
A persistent feeling of heaviness, pressure, or dull pain in the lower abdomen or pelvic area can be another warning sign. It may not seem severe at first, and it may even resemble regular menstrual cramps.
However, if the discomfort:
- Lasts for weeks
- Is unrelated to your period
- Spreads to the lower back
- Interferes with daily activities
then it is important to bring it up during a checkup.

5. Bleeding After Menopause
Any vaginal bleeding after menopause is considered abnormal, even if it happens only once or is very light. This is one of the clearer signs that should be assessed promptly.
Some women think it may be caused by dryness or age-related tissue changes. Even so, major health guidelines recommend seeking medical advice right away if postmenopausal bleeding occurs.
6. Frequent Urination or Urgency
Changes in urination can sometimes be linked to pelvic or cervical issues. Possible symptoms include:
- Needing to urinate more often than usual
- A strong urge to urinate with little output
- Burning or discomfort while urinating
- Symptoms that feel like a urinary tract infection but do not fully improve
Although this sign is not always discussed early, it can appear as cervical problems progress and should not be ignored if it persists.
7. Unexplained Fatigue
Ongoing tiredness can have many causes, but extreme or persistent fatigue that does not improve with rest may be part of a larger health concern.
Pay attention if you feel:
- Drained despite sleeping well
- Unusually low in energy without a clear reason
- Increasingly exhausted along with other symptoms on this list
Fatigue on its own may not point to a single condition, but when combined with other changes, it becomes more meaningful.
8. Lower Back Pain or Leg Discomfort
Back pain is very common, which is why this symptom is often overlooked. Still, lower back pain that has no obvious explanation, such as poor posture or muscle strain, may sometimes be connected to pelvic health concerns.
In some cases, women also notice:
- Aching that extends into the legs
- Swelling in one leg
- Ongoing discomfort without a clear cause
If this continues and does not improve, it is worth raising during a routine exam.
9. Bloating or Changes in Bowel Habits
Digestive symptoms can also be part of the picture. These may include:
- Persistent bloating
- A feeling of fullness
- Constipation
- Noticeable changes in bowel habits that do not improve with diet changes
By themselves, these issues are common and often harmless. But when they happen together with pelvic symptoms, they provide valuable information for your healthcare provider.
Quick List of the 9 Warning Signs
For easy reference, here are the nine early signs again:
- Unusual vaginal bleeding
- Changes in vaginal discharge
- Pain or discomfort during intercourse
- Persistent pelvic pain or pressure
- Bleeding after menopause
- Frequent or urgent urination with discomfort
- Unexplained fatigue
- Lower back pain or leg discomfort or swelling
- Ongoing bloating or bowel changes
These symptoms do not automatically mean cervical cancer. Many overlap with other common health conditions. That is why professional evaluation is so important.

What You Can Do Right Now
Small, practical steps can help you stay informed and in control of your health.
1. Track Your Symptoms
Use your phone, a notes app, or a calendar to record:
- Dates
- Type of symptom
- Severity
- Any patterns or triggers
Try to keep notes for at least two weeks if symptoms continue.
2. Stay Up to Date on Screenings
If you are due for a pelvic exam, Pap test, or HPV test, schedule it. Many guidelines recommend beginning Pap screening around age 21 and continuing at intervals advised by your doctor, often every 3 to 5 years depending on age and test type.
3. Ask About the HPV Vaccine
If you are in the eligible age group, speak with your healthcare provider about the HPV vaccine. In many guidelines, vaccination may be considered up to age 45. It helps protect against the virus responsible for most cervical cancer cases.
4. Practice Safer Sex
Reducing exposure to HPV and other infections matters. Helpful habits include:
- Using protection
- Being aware of partner history
- Having open conversations about sexual health
5. Avoid Smoking
Smoking can weaken the body’s ability to handle certain infections, including those linked to cervical changes. Quitting or avoiding tobacco is an important preventive step.
6. Prepare for Medical Visits
Before your appointment, write down questions such as:
- How do my symptoms compare with normal body changes?
- What screening schedule is best for my age and history?
- Should I have additional testing based on what I am experiencing?
These actions are not about diagnosing yourself. They are about improving awareness and supporting prevention.
When to Contact a Healthcare Provider
If any of these symptoms last longer than two weeks, feel different from your usual experience, or concern you in any way, contact your doctor. Do not wait for symptoms to become severe before speaking up.
Early attention can make a meaningful difference. Knowing your body, noticing unusual patterns, and staying current with cervical screening are some of the best ways to protect your long-term health.