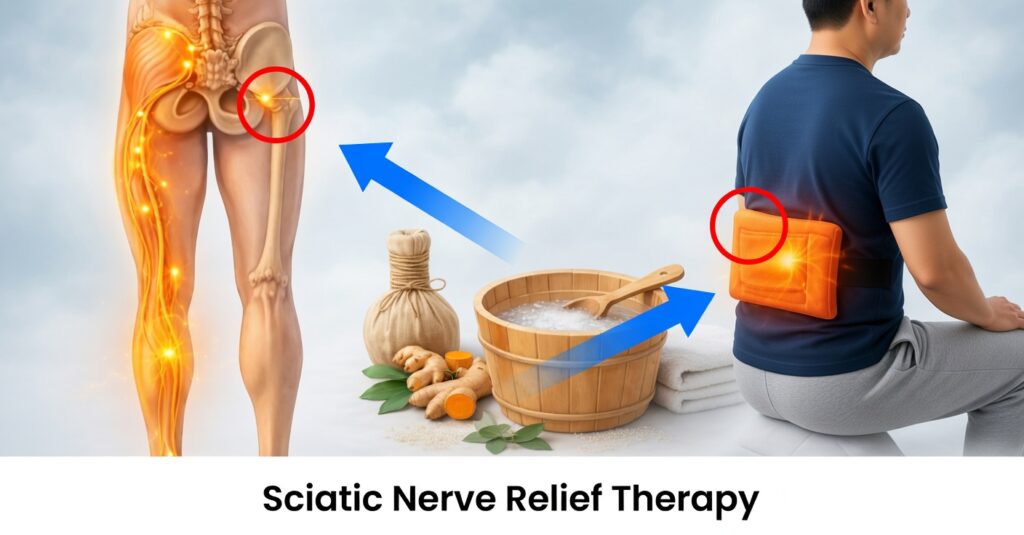
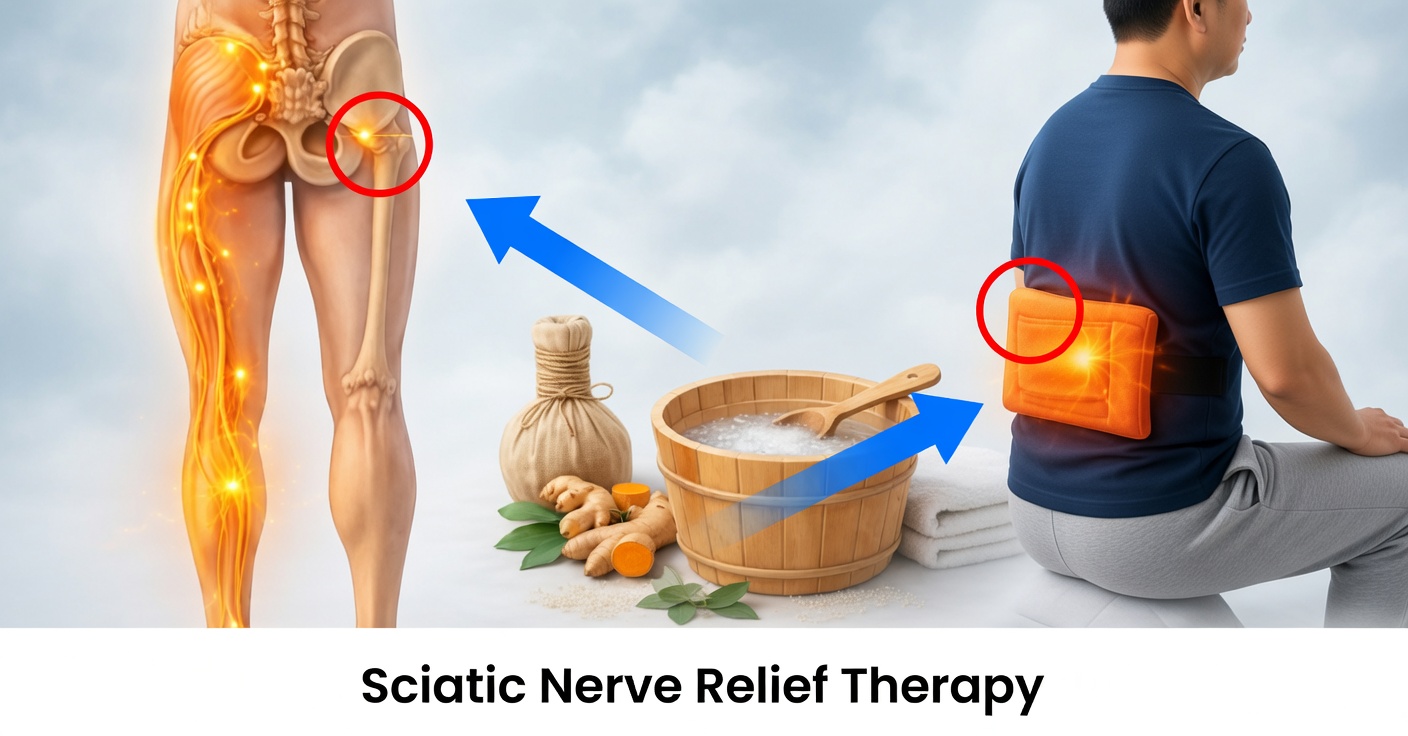
Inflamed Sciatic Nerve: Symptoms and Natural Relief
An inflamed sciatic nerve—often called sciatica—is one of the most frequent reasons for pain in the lower back and buttocks. It may begin as a mild ache in the lumbar area and, over days, turn into a sharp, burning, or electric pain that travels through the buttock and down the leg. In more intense cases, it can make walking, sitting, sleeping, and even simple daily tasks difficult.
Many people search for ways to “reduce inflammation in the sciatic nerve” as fast as possible. However, the real priority is understanding why the irritation started and what you can do to relieve pressure on the nerve. This guide explains the main symptoms of sciatica, common causes, warning signs, and natural support strategies you can use alongside professional care (not as a replacement for medical evaluation when needed).
What Is the Sciatic Nerve?
The sciatic nerve is the longest and one of the thickest nerves in the body. It originates from the lower spine (lumbar and sacral regions), passes through the buttocks, and runs down the back of the leg all the way to the foot. It is responsible for both sensation and motor function in parts of the leg.
When this nerve is compressed or irritated—either near its roots in the spine or along its path in the buttock—the characteristic pain of sciatica appears.
Common Causes of an Inflamed Sciatic Nerve
Sciatic pain rarely appears “out of nowhere.” In most cases, there is some form of compression, irritation, or tension affecting the nerve or its roots. Frequent triggers include:
- Changes in the intervertebral discs, such as bulging or degeneration that irritates nearby nerve roots.
- Deep gluteal muscle tension, especially in the piriformis muscle.
- Prolonged poor posture, such as many hours sitting or working with poor ergonomics.
- Sedentary lifestyle, with stiff hips and tight hamstrings.
- Improper lifting technique or overloading the back with heavy objects.
- Repetitive movements, in manual work or sports without proper recovery and muscle balance.
- Excess body weight, which can increase mechanical stress on the lower back.
A common pattern is a “cycle” of tension and pain: it hurts → you move less → muscles tighten further → pressure on the nerve increases → pain worsens.
Symptoms of an Inflamed Sciatic Nerve
Sciatica symptoms can range from mild and occasional to intense and disabling. Typical signs include:
- Pain in the lower back (lumbar area).
- Pain that radiates through one buttock and down one leg (usually only on one side).
- A burning or “hot” sensation along the nerve path.
- Sensations like electric shocks, stabbing, or shooting pain.
- Tingling, pins-and-needles, or numbness.
- Discomfort or pain after sitting for a long time.
- Pain when standing up, bending, or changing position.
Symptoms Suggesting More Significant Nerve Involvement
Some symptoms may indicate more notable nerve irritation:
- Weakness in the leg or foot.
- Difficulty bearing weight on the affected leg or walking normally.
- Marked loss of sensation in parts of the leg or foot.
As a general clue: when pain travels beyond the knee, it often points to clearer involvement of the sciatic nerve pathway.
Red-Flag Symptoms: When to Seek Immediate Medical Care
You should seek urgent medical evaluation if any of the following occur:
- Significant loss of strength in the leg or a “foot drop” (difficulty lifting the front of the foot).
- Severe or rapidly worsening numbness.
- Major difficulty walking or staying balanced.
- Problems controlling bladder or bowel function (incontinence or inability to void).
These can be signs of serious nerve compression and require prompt medical attention.
Natural Ways to Ease Sciatic Nerve Pain
(Supportive options for mild to moderate cases)
The strategies below may help when symptoms are mild or moderate, or as part of a broader plan supervised by a health professional. If pain is intense, keeps coming back, or lasts for weeks without improvement, it is safer to get a proper assessment.
1) Therapeutic Heat to Relax Tight Muscles
Heat can loosen tight muscles in the lower back and gluteal area, which may be adding pressure to the sciatic nerve.
How to use heat:
- Apply a warm compress or heating pad for 15–20 minutes.
- Repeat 2–3 times per day.
- Avoid placing heat directly on bare skin—use a thin cloth or towel as a barrier.
2) Gentle Movement (Avoid Complete Bed Rest)
Staying completely still for days often worsens stiffness and delays recovery. The goal is to keep moving in a controlled way, without provoking sharp pain.
Simple guideline:
- Take easy walks of 10–15 minutes, once or twice a day, as tolerated.
- Avoid sudden twisting movements, jumping, or lifting heavy objects while pain is present.
3) Targeted Stretching (Step by Step)
Perform these stretches slowly, without bouncing, and stop if you feel sharp or shooting pain.
Piriformis (Gluteal) Stretch
- Lie on your back.
- Cross the affected leg over the other so that the ankle rests on the opposite knee.
- Gently bring the lower knee toward your chest.
- Hold for 20–30 seconds while breathing calmly.
- Repeat 3 times.
Knee-to-Chest (Lower Back Stretch)
- Lie on your back with both knees bent.
- Bring one knee toward your chest, using your hands if needed, without forcing.
- Hold for about 20 seconds, then switch legs.
- Repeat 2–3 rounds on each side.
4) Strengthening the Core and Lower Back
(Key for preventing future flare-ups)
Weak abdominal and gluteal muscles can increase strain on the lumbar spine. Start with low-impact exercises:
- Glute bridge: 8–12 repetitions, 2–3 sets.
- Bird-dog (opposite arm and leg extension on hands and knees): 6–10 controlled repetitions per side.
- Modified plank (for example, on knees): hold 10–20 seconds, as long as it does not worsen pain.
Try to perform these exercises about three times per week, focusing on good form and controlled movement rather than intensity.
5) Warm Baths and Mineral Salts for Relaxation
Warm water can ease muscle tightness and reduce the sensation of rigidity around the lower back and glutes.
How to do it:
- Take a warm (not scalding) bath for 15–20 minutes.
- If you use Epsom salts or similar products, follow the instructions on the label.
6) Supportive Herbal Infusion (Optional)
Some people like to use simple kitchen ingredients as a general supportive infusion. This is not a cure for sciatica but may complement other measures.
Example recipe:
- 1 cup of hot water
- 1 slice of fresh ginger
- 1 teaspoon of turmeric
- A small pinch of black pepper
If you have gastritis, take blood thinners, are pregnant, or live with chronic health conditions, check with your healthcare provider before using such infusions regularly.
Postures and Positions That Often Help
Adapting your sleeping and sitting posture can reduce pressure on the lumbar region and sciatic nerve:
- Sleeping on your side with a pillow between your knees.
- Sleeping on your back with a pillow under your knees to slightly flex the hips.
- Avoiding sleeping on your stomach if it increases pain.
- If you work at a desk: stand up every 40–50 minutes, walk for 1–2 minutes, and reset your posture.
How Long Does Sciatica Take to Improve?
Recovery time varies depending on the underlying cause, your daily habits, and how consistently you follow treatment and self-care strategies. In mild cases, many people experience noticeable relief within 2 to 6 weeks with proper care.
If you do not see clear improvement, if the pain greatly limits your daily activities, or if episodes keep returning, it is advisable to seek a professional evaluation to identify the root cause and adjust your treatment plan.
Tips to Help Prevent Future Sciatic Pain
- Maintain a healthy body weight to reduce stress on the lower back.
- Strengthen your core, including abdominal and gluteal muscles.
- Reduce prolonged sitting: stand up, walk, and stretch regularly.
- Lift objects by bending your knees and keeping the load close to your body.
- Optimize your workstation ergonomics: chair height, screen level, and lumbar support.
- Wear supportive footwear if you spend many hours standing or walking.
Conclusion
An inflamed sciatic nerve can be extremely uncomfortable, but often improves when you reduce pressure on the nerve through a combination of heat, gentle movement, targeted stretching, strengthening exercises, and better posture habits. The aim is not only to “decrease inflammation,” but to address the mechanical and lifestyle factors that are irritating the nerve in the first place.
If your pain persists, worsens, or is accompanied by red-flag symptoms (marked weakness, changes in bladder or bowel control, severe or spreading numbness), seek professional medical guidance for a thorough evaluation.
Important notice: This article is for informational purposes only and does not replace professional medical advice, diagnosis, or treatment. If you experience severe or persistent symptoms, consult a qualified healthcare provider.