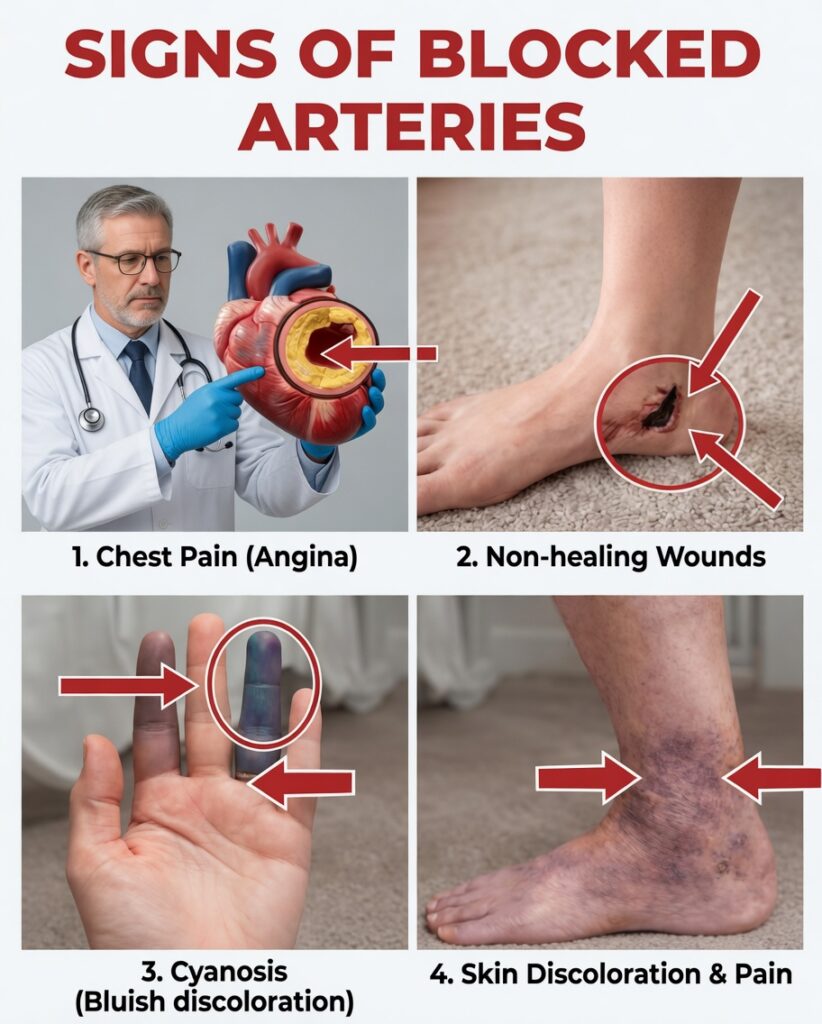
Slow-Healing Foot Wounds or Constantly Cold Feet Could Be Quiet Signs of Clogged Arteries
Foot sores that take a long time to heal—or feet that feel cold all the time—can be subtle warnings of narrowed or blocked arteries. Learning to spot these early signs may help you act before the condition gets worse.
Have you ever noticed leg pain when walking, persistently cold feet, or unusual changes in the skin on your feet? Many people brush these off as simple fatigue, aging, or standing too long. But in some situations, these symptoms can point to a more serious issue: reduced blood circulation in the legs.
When blood flow decreases, tissues receive less oxygen. Over time, this can affect mobility, muscle health, and even heart health. The encouraging part is that the body often sends warning signals well before things become severe. Recognizing them early can make a meaningful difference.
Let’s break down the most important signs to watch for.
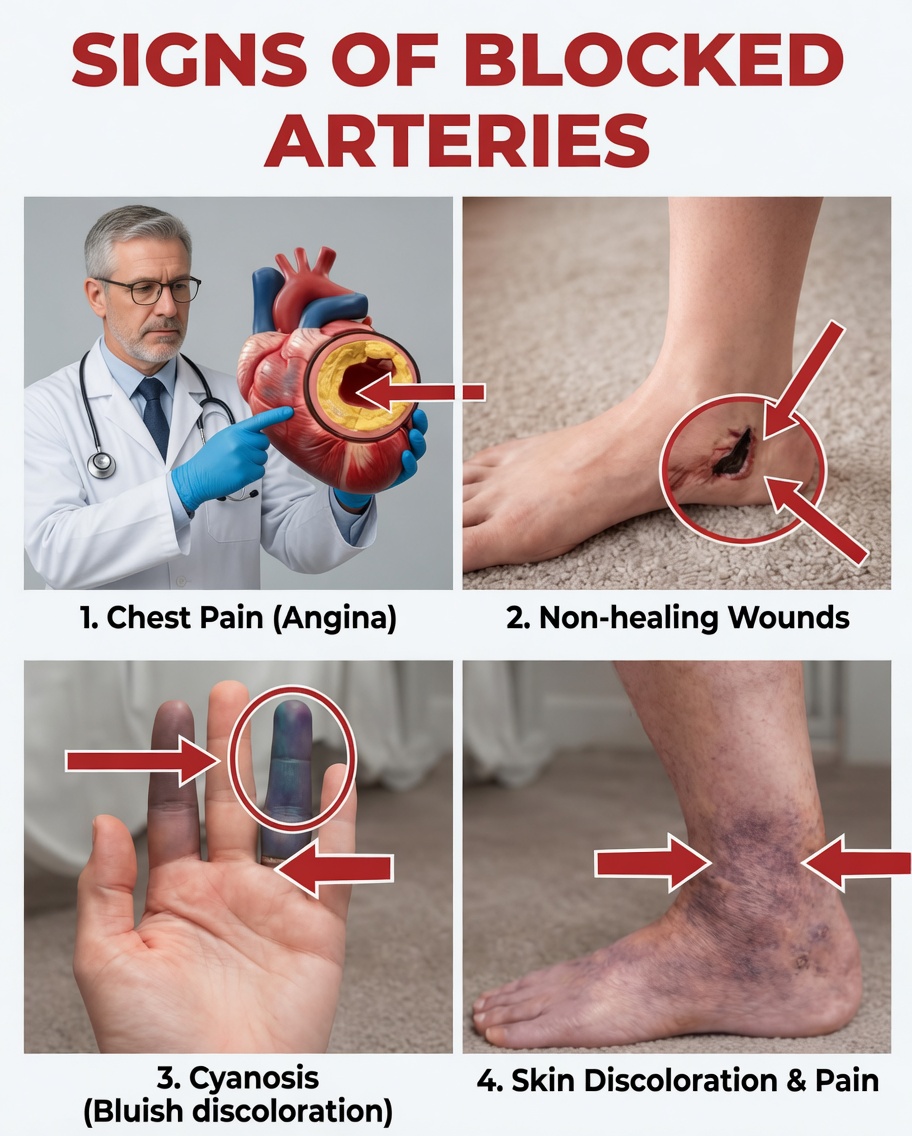
What Are Blocked Arteries in the Legs?
Blocked arteries in the legs are commonly linked to Peripheral Artery Disease (PAD). PAD develops when fatty deposits (plaque) build up inside arteries, narrowing the passageway that blood uses to travel.
This condition is more frequent in adults over age 50 and is often associated with:
- Smoking
- Diabetes
- High blood pressure
- High cholesterol
In many cases, symptoms start mildly, so people may not realize anything is wrong. That’s why paying attention to changes in your legs and feet matters.
Why Do Symptoms Often Start in the Legs?
The arteries in your legs are farther from the heart. When circulation begins to decline, feet and legs tend to show the earliest effects.
The calf and thigh muscles require significant oxygen—especially when you walk. If narrowed arteries can’t deliver enough blood, discomfort and other symptoms may appear.
Below are key warning signs that may suggest reduced circulation.
1. Leg Pain While Walking That Improves With Rest
One of the most typical signs is pain, cramping, heaviness, or tightness in the calves, thighs, or buttocks during walking.
This discomfort often:
- Starts after walking a certain distance
- Eases when you stop and rest
It happens because active muscles need more oxygen, but restricted arteries can’t meet that demand.
2. Cold Feet or Cold Lower Legs
If your feet feel cold even in warm weather, it may reflect limited blood flow.
Some people notice:
- One foot colder than the other
- Toes that feel cold to the touch
- Skin that looks unusually pale or slightly bluish
3. Wounds or Sores That Heal Slowly
Small cuts, blisters, or cracked skin usually heal relatively quickly. When circulation is reduced, healing may slow down significantly.
Common signs include:
- Sores that stay open for weeks
- Heel cracks that don’t improve
- Minor injuries that seem unusually “stubborn”
Without adequate oxygen and nutrients delivered by blood, the body struggles to repair tissue.
4. Changes in Skin Color or Texture
Your skin can reflect circulation problems. Possible changes include:
- Legs that look paler or unusually shiny
- Toes turning bluish or purplish
- Skin becoming thinner or more fragile
Some people also experience reduced hair growth on the legs, making the skin look smoother than usual.
5. A Weak Pulse in the Feet
Clinicians often check pulses around the ankles and feet to evaluate blood flow.
When arteries narrow, the pulse may become:
- Very faint
- Difficult to detect
This can be hard to assess on your own, but it’s an important finding during routine medical exams.
6. Numbness or Tingling in the Toes
Reduced blood flow can trigger sensations such as:
- Tingling
- Burning
- Numbness
Nerves rely on oxygen to function properly. If they’re not getting enough blood supply, these sensations may occur.
7. Leg or Foot Pain Even at Rest
In more advanced stages, some people develop pain in the feet or legs even while resting, often worse at night.
Sometimes the pain improves when the legs hang down off the bed, because gravity helps blood reach the feet. This may signal significantly impaired circulation and should be evaluated by a healthcare professional.
How Leg Artery Blockages Relate to Heart Health
Blocked arteries in the legs aren’t only a local issue. They can be a sign of atherosclerosis, a process that affects blood vessels throughout the body.
That means the same underlying factors impacting leg circulation may also increase risk to the heart and brain. This is a major reason early recognition is so important.
Risk Factors That Increase the Likelihood
Certain conditions and habits raise the chance of developing PAD and arterial narrowing, including:
- Smoking
- Diabetes
- High blood pressure
- High cholesterol
- Family history of cardiovascular disease
- Age over 50
If you have one or more of these risk factors, it’s wise to pay close attention to any new or persistent changes in your legs and feet.
Everyday Habits That Support Better Circulation
Simple daily choices can help support vascular health:
- Move regularly: daily walking can encourage better blood flow.
- Eat a heart-healthy diet: prioritize vegetables, fruits, whole grains, nuts, and omega-3-rich fish.
- Avoid tobacco: quitting smoking is one of the most impactful steps to protect your arteries.
- Listen to your body: persistent symptoms should be discussed with a qualified healthcare professional.
When to Seek Medical Care
Seek medical attention promptly if you notice:
- Sudden, severe leg pain
- A foot that becomes very cold or pale abruptly
- Open wounds with signs of infection
- Symptoms that worsen quickly
Conclusion
Blocked arteries in the legs and feet often begin with quiet clues: pain while walking, cold feet, skin changes, numbness, or slow-healing wounds. While these signs can seem minor, they may indicate reduced circulation and broader cardiovascular risk.
Noticing early warning signs, adopting healthier habits, and getting medical guidance when needed are practical steps toward protecting long-term vascular health.
Disclaimer: This article is for educational purposes only and does not replace professional medical advice. Always consult a qualified healthcare provider if you have concerns or persistent symptoms.